Month: November 2013
You be the judge
Jann Bellamy recently recapped her experience attending a meeting sponsored by her local Healing Arts Alliance. As you re-read her article pay particular attention to the language used by the Alliance to describe themselves and the treatments they offer. For me, there is one word that really stands out. It is emblematic of the attitude of the complementary and alternative medicine community....
Happy Thanksgiving!
We celebrate Thanksgiving Day in the U.S. on the fourth Thursday in November. Because I live in the U.S. and Thanksgiving falls on my regular blogging day this year, I get the day off. On this Thanksgiving Day, I am thankful for the cornucopia of blog fodder coming up as we move toward the end of 2013 and into 2014. The Bravewell...
The FDA and Personalized Genetic Testing
The company 23andMe provides personal genetic testing from a convenient home saliva sample kit. Their home page indicates that their $99 genetic screening will provide reports on 240+ health conditions in addition to giving you information on your genetic lineage. The benefits, they claim, are that you will learn about your carrier status and therefore the risk of passing on genetic diseases to your...
New Cholesterol Guidelines
On November 15, the American College of Cardiology and the American Heart Association released an updated guideline for the use of statins to prevent and treat atherosclerotic cardiovascular disease (ASCVD). The full report is available online. It has already generated a lot of controversy. The news media have characterized it as a “huge departure” from previous practice and have trumpeted that it...

“Low T”: The triumph of marketing over science
A man on TV is selling me a miracle cure that will keep me young forever. It’s called Androgel…for treating something called Low T, a pharmaceutical company–recognized condition affecting millions of men with low testosterone, previously known as getting older. —The Colbert Report, December 2012 And now for something completely different…sort of. After writing so much about the latest developments in...
A Rational Approach to Managing Acute Pain in Children
Pain is one of the most common reasons for a parent or caregiver to seek medical attention for their child. Children experience pain for a wide variety of reasons, many that are similar to if not exactly the same as causes of adult pain, but historically pediatric patients have been grossly undertreated. I am 37-years-old and, sadly, if I had undergone a...
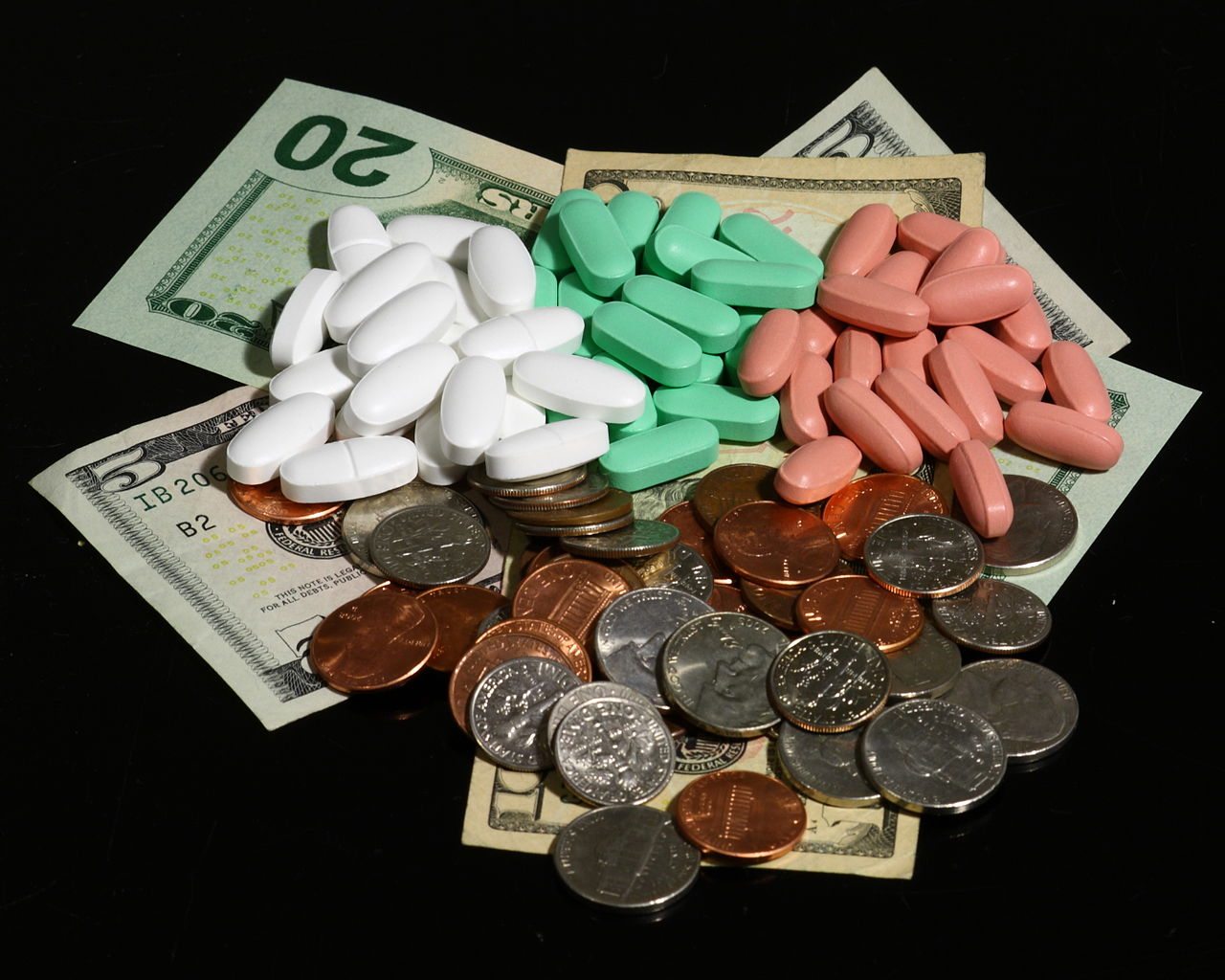
Do vitamins prevent cancer and heart disease?
The US Preventive Services Task Force has released an update on vitamin and mineral supplements to prevent heart disease and cancer. The evidence was not good and did not support taking vitamins as "nutritional insurance."

Faith Healing: Religious Freedom vs. Child Protection
We have written a lot about people who reject science-based medicine and turn to complementary/alternative medicine (CAM), but what about people who reject the very idea of medical treatment? Faith healing is widely practiced by Christian Scientists, Pentecostalists, the Church of the First Born, the Followers of Christ, and myriad smaller sects. Many of these believers reject all medical treatment in favor...
The Burzynski Empire strikes back
You might have noticed that I was very pleased last Friday, very pleased indeed. Given the normal subject matter of this blog, in which we face a seemingly-unrelenting infiltration of pseudoscience and quackery into even the most hallowed halls of academic medicine, against which we seem to be fighting a mostly losing battle, having an opportunity to see such an excellent deconstruction...

