Year: 2014
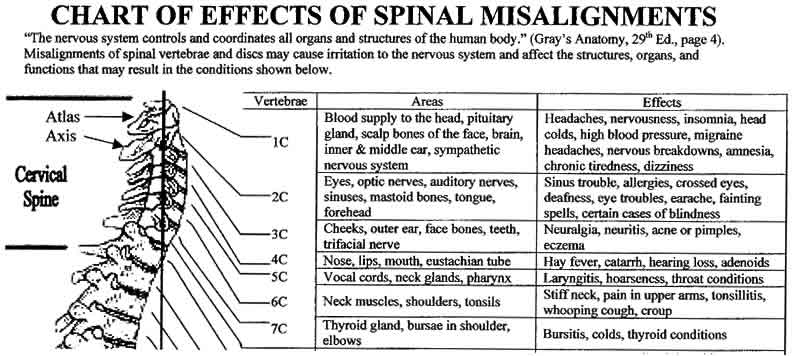
Questions and Answers about Chiropractic: The Bottom Line
I am often asked, “What do chiropractors do?” That’s not an easy question to answer. The answer is usually expected to be, “They treat back trouble.” But as alternative medicine practitioners, chiropractors do a lot of things, and they treat a variety of ailments, based largely on a scientifically-invalid vertebral subluxation theory which proposes that nerve interference resulting from a misaligned vertebra...
Ebola conspiracy theories: Same as it ever was
Does anyone remember the H1N1 influenza pandemic? As hard as it is to believe, that was five years ago. One thing I remember about the whole thing is just how crazy both the antivaccine movement and conspiracy theorists (but I repeat myself) went attacking reasonable public health campaigns to vaccinate people against H1N1. It was truly an eye-opener, surpassing even what I...

Placebo Speculations
I have a new term to add to the English language, ebolasmacked, a derivative of the British term gobsmacked. Ebolasmacked defines my life the last few weeks since Ebola, or at last preparations for Ebola, have taken a huge bite out of my time with many interesting twists and turns. I think this is maybe the 9th outbreak (HIV, MERS, SARS, Legionella,...
Connecticut “modernizes” naturopathic scope of practice
Naturopathy has been legal in Connecticut for almost 90 years, but with a scope of practice limited to counseling and a few treatments like physiotherapy, colonic hydrotherapy and “natural substances.” There was no specific authority to diagnose and treat. All of that changed on October 1, 2014, courtesy of the Connecticut legislature, which, in the words of the American Association of Naturopathic...
Neuro-Acupuncture and Stroke
On the home page of Zhu’s Neuro-Acupuncture Center there is a video relaying a testimonial of how scalp acupuncture helped a patient recover from acute stroke. The use of testimonials is very common in the promotion of dubious health treatments. A personal story and endorsement is psychologically more compelling than dry data. Testimonials are completely unreliable, however, and in fact I would...
Does the Movie Fed Up Make Sense?
The 2014 film Fed Up is an advocacy documentary. Its message: There is a worldwide epidemic of obesity. It is endangering our children. Increased sugar consumption is responsible. The food industry is responsible for our increased sugar consumption because it puts hidden sugar in processed foods, bombards us with advertising, favors profits over health, and lobbies against regulation. The government is responsible...
Andrew Wakefield, the MMR, and a “mother warrior’s” fabricated vaccine injury story
As the time came to do my usual weekly post for this blog, I was torn over what to write about. Regular readers might have noticed that a certain dubious cancer doctor about whom I’ve written twice before has been agitating in the comments for me to pay attention to him, after having sent more e-mails to me and various deans at...
Brain-Based Learning, Myth versus Reality: Testing Learning Styles and Dual Coding
Ed. Note: Today we present a guest post from Josh Cuevas, a cognitive psychologist and assistant professor in the College of Education at the University of North Georgia. Enjoy! Breaking the cycle Since early on in graduate school when I began studying cognition, I’ve followed the learning styles movement because it was such a powerful phenomenon. It took hold rapidly, seemingly overnight,...
Delaying School Start Times for Sleep Deprived Teens
In August of this year, a new policy statement from the American Academy of Pediatrics was published which tackled the widespread problem of insufficient sleep in our adolescent population. They even went so far as to label insufficient sleep as “one of the most common, important, and potentially remediable health risks in children.” The statement, which gave a number of recommendations on...
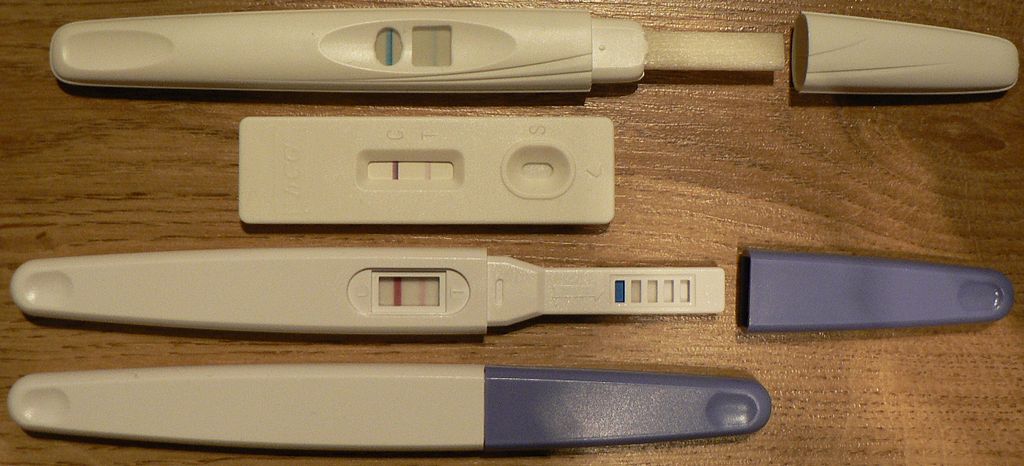
Naturopathy vs. Science: Infertility Edition
This is another post in the naturopathy versus science series, where a naturopath’s advice is assessed against the scientific literature. It’s Naturopathic Medicine Week in the United States, so it’s time for another look at the alternative medicine practice that a friend of the blog likes to call the One Quackery to Rule them All. Naturopathy is an oddity among alternative medicine,...

