Hormone Replacement Therapy for Menopausal Symptoms: Setting the Record Straight
Whether you call them hot flashes or “power surges,” the symptoms of menopause can be very distressing. They were routinely treated with hormone replacement therapy (HRT) until the Women’s Health Initiative study in 2002 persuaded many patients and doctors to abandon that treatment. The results of that study were misunderstood by some and questioned by others, and there continues to be confusion...
The “Incoherent Mess” That Is Homeopathy: Old and New Insights
Back in 1943 a Dutch physician, David Karel de Jongh, wrote a PhD dissertation on homeopathy. It was based on his experience working in a homeopathic hospital and on all the published information he could find, and was highly critical of homeopathy. It was an impressive opus, with over 200,000 words. It is way too long for the average reader to wade...
Sharks Get Cancer, Mole Rats Don’t: Clues to Understanding Cancer
We think of cancer as caused by mutations. Mutations are necessary, but not sufficient, to cause cancer. New research indicates that it’s the body’s response to mutant cells that determines whether cancer will develop. James S. Welsh, MD, a radiation oncologist and researcher, has written a book on the immunology of cancer, Sharks Get Cancer, Mole Rats Don’t: How Animals Could Hold...
Questioning the Evidence for Breastfeeding
Is breast best? Yes, but it's really not much better than formula in the United States. The better you account for confounding factors, the more benefits of breastfeeding disappear.
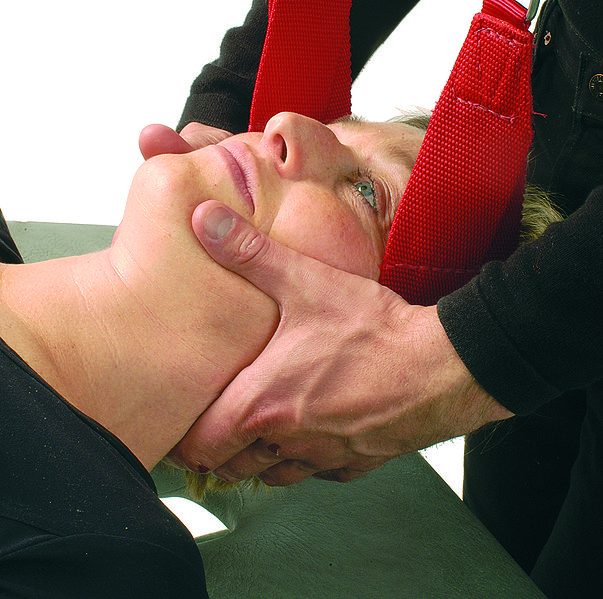
When Headaches Are a Pain in the Neck: Spinal Manipulation vs. Mobilization for Cervicogenic Headache
NOTE: Today we offer a double feature on the treatment of cervicogenic headache. My article is about a study that compared manipulation to mobilization; it is followed by retired chiropractor Sam Homola’s guest article on manipulation for cervicogenic headache. The two posts complement each other and also complement my post from last week on the possible risk of stroke with neck manipulation....
Chiropractic and Stroke: No Evidence for Causation But Still Reason for Concern
Can neck manipulation (by chiropractors or by other practitioners) cause strokes? Many of us think it can, but definitive proof is lacking. A recently published study looked at the available evidence. A systematic review found a small association between stroke and chiropractic care but concluded that the association was spurious and that there was no evidence for causation. My colleagues and I...
Carotid Artery Stenosis: Surgery, Stent, or Nonsurgical Stroke Prevention?
The carotid artery in the neck is a common site of atherosclerosis. As plaque builds up, it leaves less room for blood flow and can cause strokes through clotting or embolization. Carotid stenosis is defined as a greater than 70% narrowing of the lumen (the space through which the blood flows in an artery). It can cause symptoms, including transient ischemic attacks...
Testing Testosterone Treatments
Ponce de Leon is said to have been looking for the Fountain of Youth when he explored Florida. That’s only a myth. Now there’s a new myth, that testosterone supplements are a Fountain of Youth for aging men. Men are urged to get their testosterone levels checked if they have any of a long laundry list of vague symptoms. Anti-aging clinics promote...
Cargo Cult Psychology
Last year I reviewed Tomasz Witkowski and Maciej Zatonski’s book Psychology Gone Wrong where they pointed out that many of psychology’s accepted beliefs and therapies were not based on good evidence. Now Witkowski has written a new book, to be published later this year, Psychology Led Astray: Cargo Cult in Science and Therapy, that is certain to ruffle a lot of feathers....


Is the Annual Physical Unnecessary?
I was approached by The Wall Street Journal to write an article for their Big Issues in Health Care debate series. The subject was “Is the annual physical unnecessary?” I was to take the “yes” side and an internist was to take the “no” side. I wrote the following article. The editor wrote me a couple of times with questions. The internist...