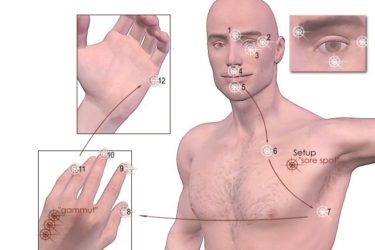
Emotional Freedom Technique – Acupuncture for the Mind
Emotional Freedom Technique is based in pseudoscience and inadequate clinical research.
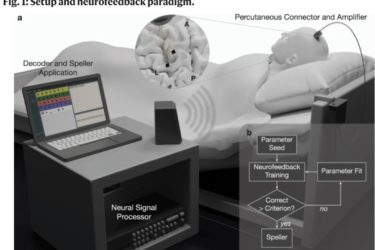
Paralyzed Patient Communicates with Brain Implant
Brain-machine interfaces continue to advance.

Facilitated Communication Is Still Pseudoscience
Facilitated communication is a harmful pseudoscientific technique that has managed to survive through rebranding and deception.
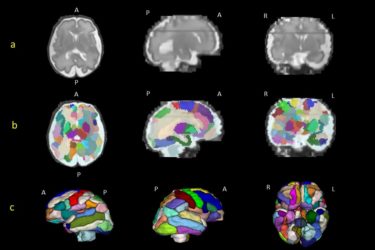
Fetal Signs of Autism
More evidence that ASD is a developmental disorder that begins in the womb.
Update on Long COVID
Recent evidence suggests the burden of long COVID is significant.

Allergy Release Technique
A dubious intervention for food allergies follows a typical pattern for such treatments.
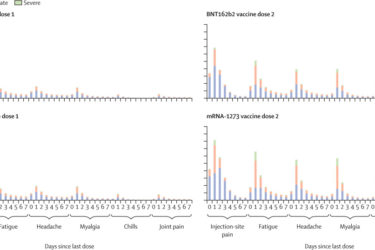
New Study – mRNA Vaccines Safe
After more than 298 million doses give, the side effects of the mRNA vaccines are minimal and transient.
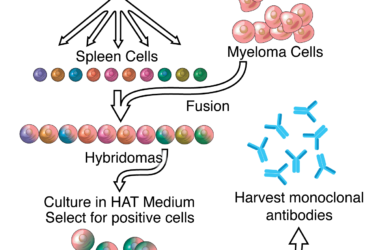
Crizanlizumab for Sickle Cell Crisis
Monoclonal antibodies to prevent sickle cell crises represents the promise and difficulties of high tech medical treatment.
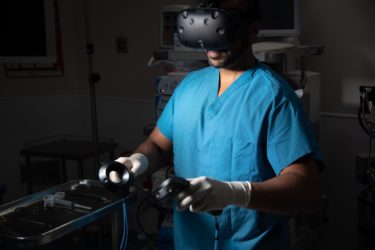
AI Medical Tutoring Systems
Using AI powered virtual training systems can be a boon to medical education and practice.

Medical Reversals – Checking the Evidence
How often are standard medical practices reversed by later high quality evidence?

