
More Evidence Raw Milk is Bad
More evidence that raw milk has no health benefit, but does carry higher health risks.

Can Air Purifiers Stop Spread of COVID-19 Virus?
Air purifiers can remove droplets and viruses from the air, but they cannot prevent the spread of COVID-19 in a mass gathering.

Homeopathy is Worthless and Not Always Harmless
More cases of homeopathic contamination remind us that it is beyond time to properly regulate this pseudoscience.
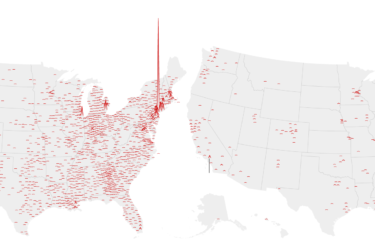
COVID-19 – The Second Wave
A second wave seems likely, but the evidence suggests our measures are working, and may even prevent a second wave.

Winning the COVID Marathon
The most important difference between the COVID-19 pandemic and all previous pandemics is the power of our science. We should acknowledge and maximize that.

Herbal Products and Pregnancy
A recent review shows that herbal products do present a potential risk during pregnancy, and should not be considered automatically safe.
COVID-19 Testing
Currently available tests for COVID-19 are imperfect but useful if used properly, with rapidly evolving research on new tests underway.

Do Masks Work?
Let's review the evidence for the effectiveness of wearing face masks during a pandemic (reprinted from NeuroLogica).

MMR is Safe and Effective
A new systematic review shows convincingly that the MMR vaccine is safe and effective.


The Coming Age of Telehealth
Telehealth is finally here. We should keep it.