
Multivitamins and Vascular Disease
Yet another massive meta-analysis shows no health benefit to routine supplementation with vitamins or minerals.
Polio Outbreak in Papua New Guinea
A recent case of polio on Papua New Guinea shows that we cannot rest until the eradication of polio is complete. Close is not good enough.

Is Gaming Addiction a Thing?
The WHO has added gaming disorder as an official ICD diagnosis, and the APA is considering adding gaming disorder to the DSM. What is gaming disorder and how should it be diagnosed?

Halotherapy – The Latest Spa Pseudoscience
Halotherapy, sitting in a salt room, is the latest spa trend, just as full of pseudoscience and false claims as we have come to expect from wellness spas.

Health Effect of Wind Turbines
What are the health effects of living close to wind turbines? The answer is, probably not much, but definitive data is elusive.
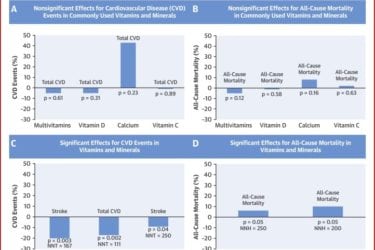
Routine Vitamin Supplementation Mostly Useless
A new meta-analysis shows no benefit from multivitamins or routine supplementation. These results should motivate users to take a fresh look at their supplementation.

Death from Cancer Quackery – Black Salve Edition
An Australian nurse dies of cancer while being treated by a cancer quack with a caustic substance known as black salve. How and why is this allowed to happen?

Essential Oils in the Ambulance
Aromatherapy with essential oils is pseudoscience, backed only with low quality studies guaranteed to show a placebo effect. Their growing popularity warns that better science education is needed.

Stem Cell Tourism Comes Home
You used to have to go to China to get ripped off by fraudulent stem cell clinics. Now you can get conned right here at home.


Independence Day!
Happy 4th to all our readers.