Category: Basic Science

Corrigendum. The Week in Review for 03/19/2017
What happened this week? Measles returns to kill. Stem cell injections blind. Lousy acupuncture studies. Fire hot. Skinny jeans are not a reason to see a chiropractor. Lesbian tendencies do not respond to homeopathy. And more.

Corrigendum. The week in review for 03/12/2017
Waiting for a vaccine-preventable infection. More lousy acupuncture studies. Medical students interested in homeopathy are not as strong at science. Water wet. TCPM consuming donkeys. What the FDA does, and doesn't do, for now.
Influenza Vaccine and Health Care Workers. More than one way to skin a literature
There are many ways to apply the medical literature. For me it starts with the premise that health care workers may not injure a human being or, through inaction, allow a human being to come to harm.

Corrigendum. The Week in Review for 02/19/2017
More poorly done acupuncture studies. Burzynski eats just desserts. Italians like homeopathy. New Jersey is going after Oregon. And more
Donald Trump versus the FDA: Is the standard of evidence for drug approval actually too low rather than too high?
All of the candidates being considered by President Trump for FDA Commissioner believe that the FDA is too strict in its standards for approving new drugs. In a commentary in Nature last week, two bioethicists argued that, at least in terms of preclinical data, the standard of evidence is actually too low. Which is correct?

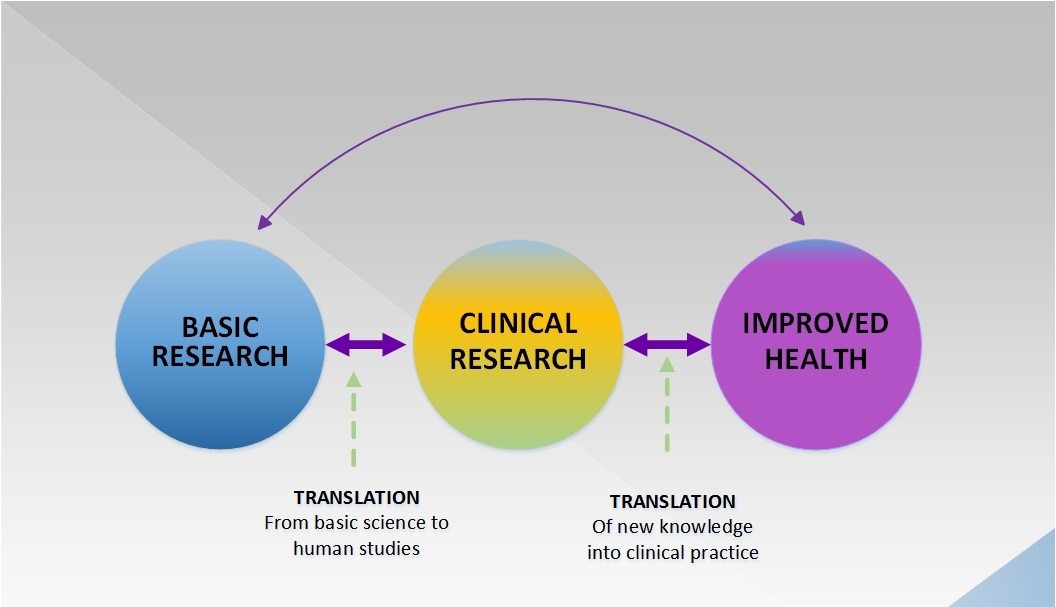
How reproducible is basic lab research in cancer biology?
Last week, a review of the reproducibility of several highly cited cancer biology papers was published. The results were mixed and demonstrate how difficult reproducing published results can be at times—and how scientists need to do better.

A review of Benecol, a plant-stanol margarine
Most nutraceuticals don't really work as advertised. For the most part, Benecol pretty much does. But is it worth it?

We still Need Better Communication on GMOs
A new PEW survey has been carried out regarding public attitudes toward genetically modified organisms (GMOs), organic food, and scientific consensus. While the numbers are better than I expected for science, they still indicate a large disconnect between scientific and public opinion on food matters. Scientists need to do better.
Phenibut Is Neither Proven Nor Safe As A Prosocial Wonder Drug
Editor’s note: With Mark Crislip away on yet another vacation, we present an inaugural guest post from Abby Campbell, a practicing MD, Ph.D and contributor at HealthyButSmart.com. Welcome Abby! On average for the past year, phenibut has been typed into google 49,500 times a month. Phenibut is a supposed wonder drug that claims to promote sociability and lessen anxiety. When people run...

Medical science policy in the U.S. under Donald Trump
The election of Donald Trump was unexpected. Given Trump's history of antivaccine beliefs and conspiracy theories, coupled with a fervor for deregulation (a fervor shared by the Republican Congress), it is reasonable to fear what will happen to medical science policy during the next four years.

