Category: Cancer

Be careful what you wish for…
A "naturopathic oncologist" on Twitter challenged me to examine the work of his two "naturopathic oncology" mentors. It did not go well...for him.

More, please! A victim of cancer quack Robert O. Young wins a $105 million settlement
Robert O. Young is a cancer quack who claims to be a naturopath who promotes what he calls "pH Miracle Living." He claims that cancer is caused by excess acid and that the way to prevent and cure cancer is to "alkalinize the blood." Two and a half years ago, he was convicted of practicing medicine without a license. Last week, a...

My Cancer Free Life: A reality series designed to promote Stanislaw Burzynski’s quackery
Stanislaw Burzynski has been selling a dubious treatment known as antineoplastons to desperate cancer patients since the late 1970s. Unfortunately, there are those who are all too willing to promote the myth of a Brave Maverick Doctor who can cure cancer. Several years ago, it was Eric Merola. Now it's Uchenna Agu, a reality TV star turned producer. He plans on making...
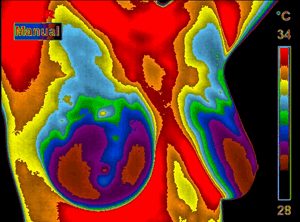
Thermography is Not Approved for Breast Cancer Screening in Canada
Breast cancer thermography is being promoted across Canada as a reliable and effective way of identifying breast tumors. There is no evidence thermography is actually capable of doing so.

Cancer disparities: It’s money that matters (along with a lot of other things)
Cancer is a complex set of diseases. I commonly discuss complexities in its biology and treatment. However, there's another layer of complexity that leads to marked disparities in cancer incidence and death rates. One major factor associated with such disparities is socioeconomic status.
A whole issue of JACM devoted to “integrative oncology” propaganda? Oh, goody.
Last week, The Journal of Alternative and Complementary Medicine published a Special Focus Issue on "integrative oncology." In reality, it's propaganda that promotes pseudoscience and the "integration" of quackery into oncology.

Crowdfunding: The fuel for cancer quackery
Ever since I first started taking notice about cancer quacks like Stanislaw Burzynski, I noticed how crowdfunding using social media and sites like GoFundMe appear to be an integral part of the business model of quack clinics. Thanks to an investigation by The Good Thinking Society published in BMJ last week, I now have a feel for the scope of the problem....
Acupuncture versus breast cancer treatment-induced joint pain: Spinning another essentially negative study
The investigators behind a recent clinical trial testing acupuncture to treat joint pain caused by aromatase inhibitors used to treat breast cancer are spinning it as a positive study. As is usually the case for acupuncture studies. It isn't

Estrogen Matters
Hormone replacement therapy in menopause is safer and more effective than we have been led to believe. A new book examines the evidence and sets the record straight.
Bad Documentary Review: Cancer Can Be Killed
Cancer Can Be Killed is a conspiracy thriller masquerading as a documentary. Don't watch it.

