Category: Clinical Trials

What the heck happened to John Ioannidis?
John Ioannidis is one of the most published and influential scientists in the world, someone whose skewering of bad medical research we at SBM have frequently lauded over the years. Then the COVID-19 pandemic hit. Since then, Prof. Ioannidis has been publishing dubious studies that minimize the dangers of the coronavirus, shown up in the media to decry "lockdowns," and, most recently,...

The Brownstein protocol is not a proven treatment for COVID-19
Dr. David Brownstein is a "holistic" physician who practices in Dr. Gorski's neck of the woods. Unfortunately, he just wrote a book promoting an unproven protocol involving vitamins, nebulized hydrogen peroxide and iodine, and intravenous ozone to treat COVID-19. There is no evidence that his protocol works, other than a very poor quality case series.
Hepatitis C Vaccine Fails Testing
A vaccine regimen intended to prevent chronic HCV infection was tested in a double-blind placebo-controlled trial. It failed. The incidence of chronic HCV infection was the same in the vaccinated group as in the placebo group.

The effectiveness of zinc and vitamin C on the duration of COVID-19 infections
Vitamin C and zinc have been heralded as treatments for colds for decades, but how well do they work against COVID-19? A new clinical trial provides the answer.

Statin Side Effects Revisited
Patients on statins frequently report muscle pain and other side effects, but controlled studies have shown side effects are not more frequent than with placebo. Why this discrepancy? A new study sheds some light.

Wim Hof, the Iceman
Wim Hof, the Iceman, is extraordinarily resistant to extreme cold. His Wim Hof Method (WHM) combines breathing exercises, cold exposure, and meditation. Hyperventilation has been shown to reduce the body's response to inflammation, but Hof's extravagant claims of health benefits are not supported by scientific evidence.

Progeria
The first drug to treat Hutchinson-Gilford Progeria, a rare and uniformly fatal rapid aging disease, has been approved by the FDA. It can prolong the life of these children by 2.5 years, but it is very expensive.
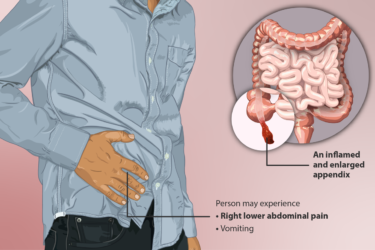
Appendicitis: Surgical vs. Medical Treatment
Surgery or antibiotics for appendicitis? This new study can help with the decision.
When Doctors Refuse to Believe Evidence
Paul Offit's new book covers the evidence for many surgeries, medications, and screening tests that have been proven ineffective and harmful yet are still being used by doctors who refuse to follow the science.

Jumping the Gun: Antibody Drugs for Covid-19
Why did the US government promise to buy a product that had failed testing?

