Category: Energy Medicine
The false dilemma of David Katz: Abandon patients or abandon science
Dr. David L. Katz is apparently unhappy with me. You remember Dr. Katz, don’t you? If you don’t, I’ll remind you momentarily. If you do, you won’t be surprised. Let me explain a bit first how Dr. Katz recently became aware of me again. Last week, I posted a short (for me) piece about something that disturbed both Steve Novella and myself,...
Amber Waves of Woo
As a pediatrician I have an opportunity to observe a wide variety of unusual and sometimes alarming parental efforts meant to help children through illness or keep them well. I have recently noticed one particular intervention that seems to be becoming more prevalent, at least in my practice. I’ve begun to see more and more infants sporting Baltic amber teething necklaces. These...

A tale of quackademic medicine at the University of Arizona Cancer Center
NCI-designated comprehensive cancer centers like the University of Arizona should provide rigorously science-based treatment. Unfortunately, magical mystical "treatments" like reiki are offered to UA patients, as I learned from a father of a child treated there.
I Visited a Chickasaw Healer and All I Got Was an Elk Sinew and Buffalo Horn Bracelet
Which headline is real? I Visited a Alchemist. As American alternative chemistry grows in popularity, I decided to experience an even older style of nontraditional transmutation of metals. I Visited an Astrologer. As American alternative astronomy grows in popularity, I decided to experience an even older style of nontraditional stargazing. I Visited a Bloodletter. As American alternative medicine grows in popularity, I...
Full of Energy
Want to know what a craniosacral treatment is actually like? How about reiki? What about Eden energy medicine – do you even know what that is? Read on, because this past Sunday afternoon I experienced all three. But first, the why and where. The local Healing Arts Alliance of the Big Bend (which is what they call the area of Florida I...
Integrative Medicine’s Collateral Damage
Integrative medicine combines the practice of medicine with alternative medicine. Proponents tend to take a paragraph or two to say this, but that is what remains when boiled down to its essence. By putting this more concise definition together with Tim Minchin’s often-quoted observation about alternative medicine, you get: integrative medicine is the practice of medicine combined with medicine that either has...
Licensing Naturopaths: the triumph of politics over science
Naturopaths shouldn’t get too excited about having a special week in their honor. The U.S. House of Representatives gave watermelons a whole month. As between naturopathy and watermelons for my good health, I’ll go with the watermelons any day. You’ll soon understand why. Today is not my usual blogging day. But when David Gorksi announced SBM’s celebration of Naturopathic Medicine Week, I...
Cranial Manipulation and Tooth Fairy Science
Tooth Fairy Science is science that studies a phenomenon that doesn’t exist. You can do studies on the Tooth Fairy; for instance, comparing how much money she leaves to kids in different socioeconomic groups. You can do studies on the memory of homeopathic water. You can do studies on the therapeutic effects of smoothing out wrinkles in the imaginary human energy field...
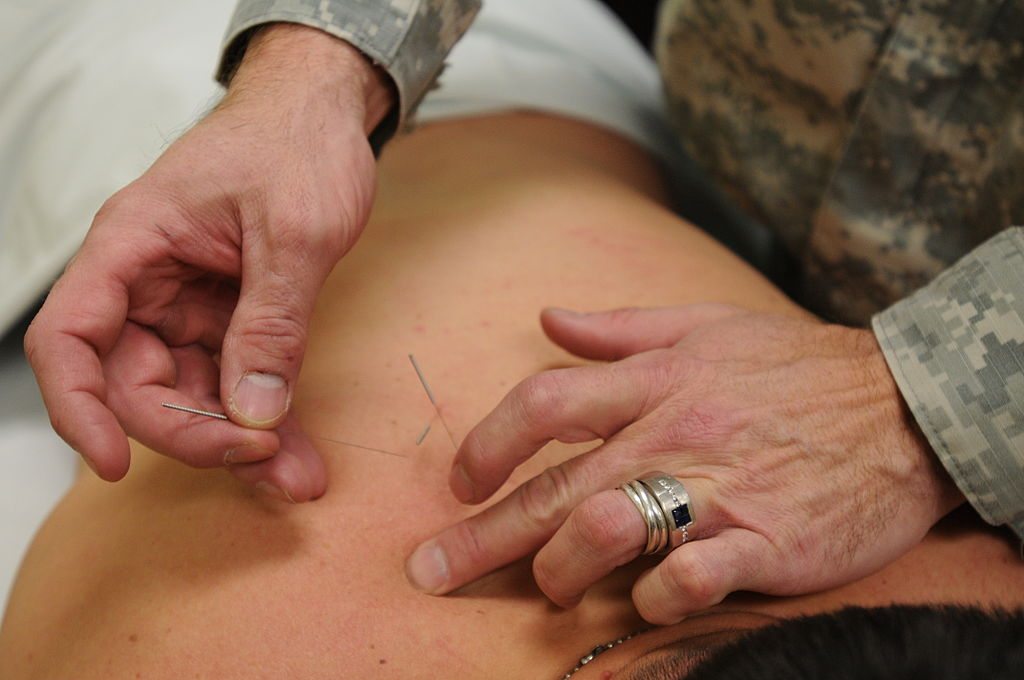
Integrative Medicine Invades the U.S. Military: Part Two
An unfortunate side effect (if you will) of states licensing of “CAM” practitioners is their ensuing insinuation of themselves into the nooks and crannies of the American health care system. Sometimes this is voluntary, such as their inclusion as providers of health care services in medical practices and other institutional settings in the form of integrative and quackademic medicine. Where voluntary action...
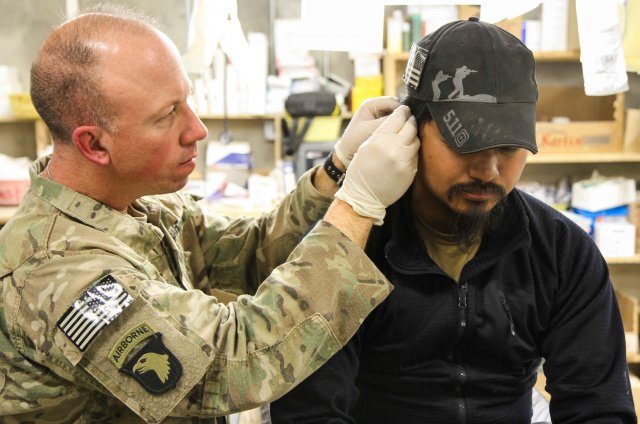
Integrative Medicine Invades the U.S. Military: Part One
Integrative medicine proponents claim superiority over physicians practicing “conventional” medicine. (Which I will refer to as “medicine” so as not to buy into integrative medicine’s implied claim that medicine can be practiced with two separate standards.) While conceding that medicine is good for treating conditions like broken arms and heart attacks, physicians who purport to practice integrative medicine argue it ignores “the...

