Category: Neuroscience/Mental Health
How We Believe
James Alcock's new book about belief is a masterpiece that explains how our minds work, how we form beliefs, and why they are so powerful. It amounts to a course in psychology and an owner's manual for the brain.

Is Gaming Addiction a Thing?
The WHO has added gaming disorder as an official ICD diagnosis, and the APA is considering adding gaming disorder to the DSM. What is gaming disorder and how should it be diagnosed?

Mosconi’s Brain Food Diet
Mosconi offers a plan to prevent and treat Alzheimer's and maximize cognitive function in everyone. She claims brain health requires a unique diet, but she fails to make her case. Some of what she says is good standard health advice, but the rest is speculative, not based on good scientific evidence, and sometimes demonstrably wrong.

Reflex Integration Therapy
Various methods of reflex integration claim benefits for autism, ADHD, brain injuries, pain, and more. They are based on speculative ideas about retained primitive reflexes. They have not been scientifically tested.
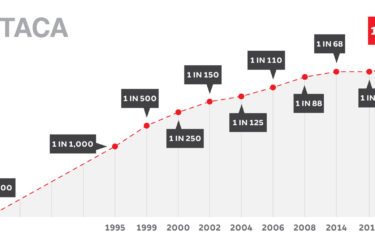
Autism prevalence increases to 1 in 59, and antivaxers lose it…yet again
Autism Awareness Month isn't as full of news stories about autism with false balance between science and antivaccine pseudoscience advocates as it was in years past. Every few years, though, when new autism prevalence figures are released, we can count on antivaxers losing it. 2018 is just such a year.

“Dr. Amy” Yasko’s Autism Protocol: Unproven, Complicated and Expensive
"Dr. Amy" Yasko isn't a real doctor and her autism protocol is unproven, complicated, and expensive. Her claims of success are contradicted by autism, nutrition, and genetics experts.
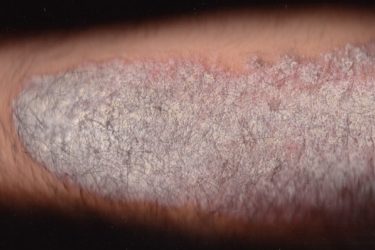
Psychodermatology?
A new specialty, psychodermatology, was invented to address the interaction of the mind and the skin. The effects of stress on the skin are not well defined, and the need for this new specialty is questionable.
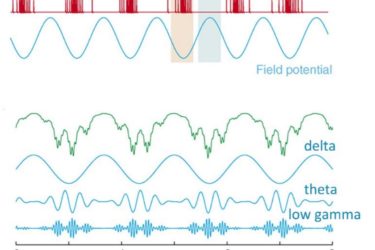
Music for ADHD?
In a recent "Ask Me Anything" on Reddit, the CEO of Brain.fm claimed his company's music can improve concentration and help with ADHD. At the very least I see such claims as highly implausible, and not something we can conclude from the existing basic science research. I have no problem with doing clinical research, and maybe we might learn something about how...

Facilitated Communication Rears Its Ugly Head Again
Facilitated communication is pure pseudoscience that was debunked almost 30 years ago, but it keeps coming back, creating new victims.

The Debate Is Over: Antidepressants DO Work Better Than Placebo
The idea that antidepressants are no more effective than placebo has been put to rest. They clearly work when used appropriately, although the effect size is not as large as the published studies have suggested.

