Category: Nutrition

A review of Benecol, a plant-stanol margarine
Most nutraceuticals don't really work as advertised. For the most part, Benecol pretty much does. But is it worth it?

Natural Medicine, Starvation, and Murder: The Story of Linda Hazzard
History is replete with doctors who practiced quackery. Here is the story of one such quack whose fasting therapy resulted in many deaths, a story that is so bizarre and horrific that it's hard to believe it really happened, but it did.

Betraying the Science on Vegan Nutrition
After the prolonged comment thread in Harriet Hall's review of this book in July, given the controversy, we were willing to consider a guest post offering another perspective. In this case, the perspective, from a dietician, is similar to Harriet's, the main difference being primarily in emphasis.

Diet and exercise versus cancer: A science-based view
Yes, diet and exercise can be useful to prevent some cancers. Unfortunately, they don't prevent all cancers, and the effect size is more modest than often represented. That's not to say that eating right and exercise aren't good. They are, for so many other reasons than cancer. Just don't view them as a panacea for preventing cancer.
Sugar Industry Research
A recent New York Times article about how the sugar industry manipulated research starting in 1965 is getting some attention. The article is largely based on a recent JAMA Internal Medicine article that reviews historical documents revealing how the Sugar Research Foundation (SRF) (based largely on revealed internal documents) put their thumb on the scale of diet research starting in 1965 in...
Oxygen water? You can’t breathe through your stomach
My exercise of choice is running. Despite the heat I’ve been having a great summer, training for the Chicago marathon. I’ve followed the training schedule fanatically since June. But it all came crashing down in one run last week when I moved from the ranks of “marathoner in training” to “injured runner”. With the sudden onset of very sharp, radiating back pain,...
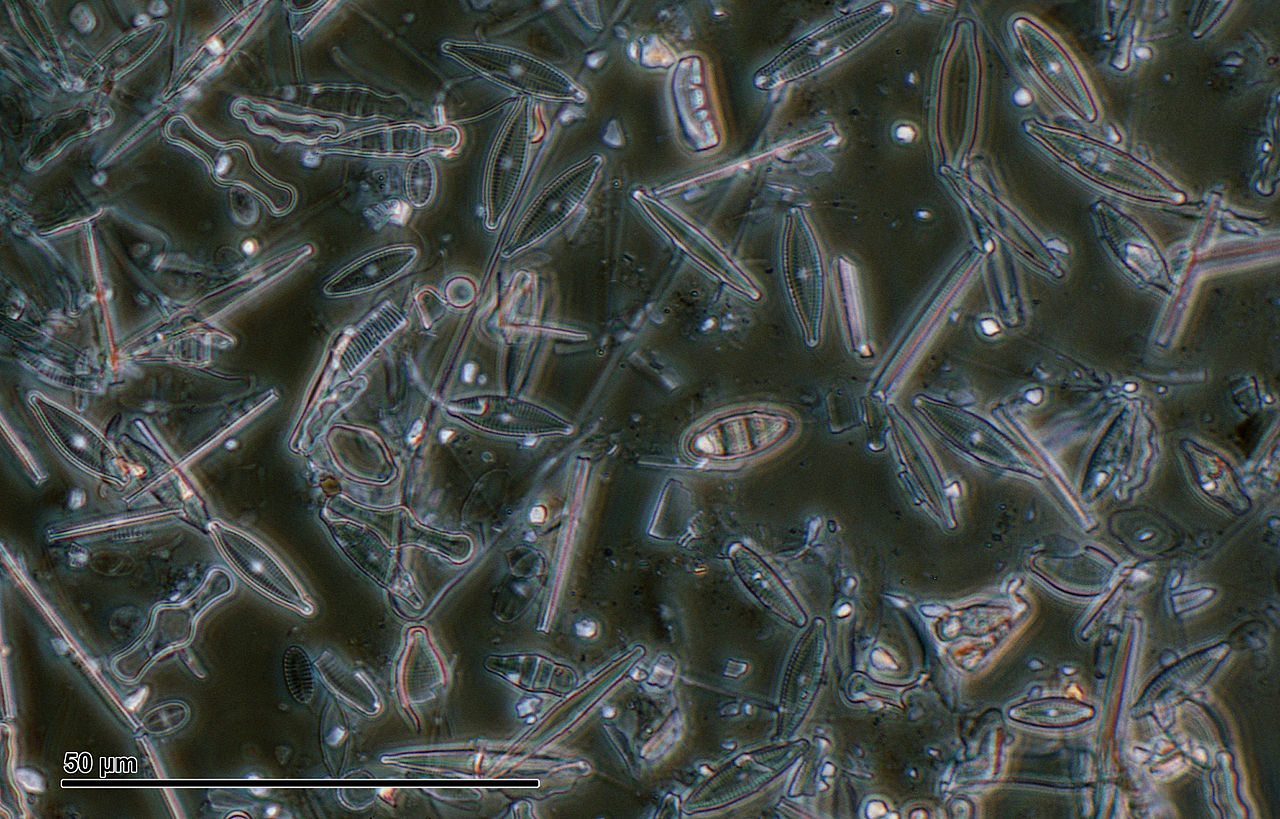
Diatomaceous Earth? No Thank You!
Diatoms are unicellular algae, one of the two major classes of the phytoplankton that constitute the bottom of the food chain in oceans and freshwater. Diatomaceous earth is a soft, siliceous sedimentary rock containing the fossilized skeletal remains of diatoms. It has been used as a bug killer: it is hypothesized that the sharp particles physically cut up the insects and also...

Vegan Betrayal: The Myths vs. the Realities of a Plants-Only Diet
NOTE: The original version of this book review was criticized for not making it clear when I was simply reporting the book’s content and when I was expressing support for one of its arguments. I have revised it to make it more clear. The additions are marked by brackets. Vegetarians come in several flavors. Ovo-vegetarians eat eggs, lacto-vegetarians eat dairy products but...
Health and Wellness Coaching: cautious optimism and some concerns
The National Consortium for Credentialing of Health & Wellness Coaches (NCCHWC) and the National Board of Medical Examiners (NBME) signed an agreement last month for the launch of a national certification for individual health and wellness coaches in the U.S. According to a joint press release, the agreement is a landmark in the efforts of a dedicated group of individuals who have...


