Category: Science and Medicine
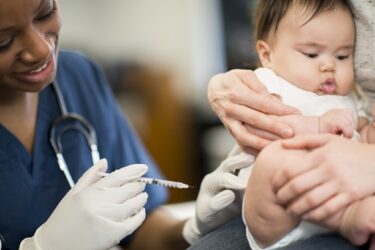
Childhood Vaccination Rates Move (Slowly) in the Right Direction
Childhood vaccination rates worldwide tanked during the first two years of the pandemic. A recently released report from the UN revealed that 2022 was better, but the improvements weren't seen everywhere. And we still have a long way to go.
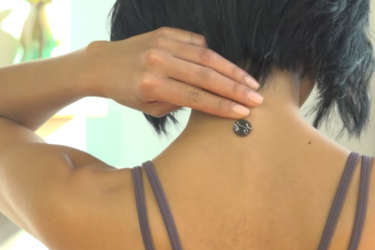
Novak Djokovic credits the TaoPatch for his success: What does the science say?
His ‘Biggest Secret’ is a tiny sticker selling for hundreds of dollars

The Grand Debunk of the antivaxxer book “Turtles All the Way Down” (part 2/10)
The second installment in debunking the antivaxxer book "Turtles All the Way Down": Chapter 2, supposedly concerned with “The Science of Adverse Events”.

Praise for Dr. Monica Gandhi
Ideally, leaders of American medicine would have had the courage to correct misinformation spread by their fellow doctors. At a bare minimum, they didn't have to lavish praise on a doctor who repeatedly polluted our COVID landscape with obvious misinformation and falsely pacified people the worst was over, when in fact the worst was yet to come.

The Grand Debunk of the antivaxxer book “Turtles All the Way Down” (part 1/10)
This book — written by "Anonymous", edited by Children's Health Defense lawyer Mary Holland and Children's Health Defense Publisher Liaison and Thinking Moms’ Revolution co-founder Zoey O’Toole, and published by "The Turtles Team" — purports to use only mainstream references to prove its points. But the book employs all the standard tropes in a master class of science denial and antivax tactics...

The return of marketing hype for “whole body scans”…now with AI!
Two decades ago, I cut my skeptical teeth countering advertising for whole body scans by companies making extravagant promises for their products. This particular medical fad faded for a while, but now it's back with a vengeance...with AI! Looking at these products, what I see is basically the quackery that is functional medicine on steroids and powered by AI.

Delabeling Penicillin Allergies: A Public Service Announcement from Science-Based Medicine
Is your child allergic to penicillin? Are you sure about that? Penicillin allergy is much less common than widely believed and there is a big push to delabel pediatric and adult patients who actually can tolerate these antibiotics.

When Doctors Have Different Standards of Evidence for the Virus and the Vaccine
817,000 Americans had already died of COVID by December 23, 2021, and 244,000 more would die the next year. Millions more survived, but were injured. These numbers could have been lower if doctors had not become defense attorneys for SARS‑CoV‑2 and prosecutors against the vaccine, and instead applied similar standards of evidence to both.

Anti-Vaccine Doctors: “Kids Don’t Need the Vaccine Because They Are Less Likely to Acquire SARS-CoV-2 and Because Most Already Had COVID-19”
Those of us who thought about vaccines before the pandemic know perfectly well that anti-vaxxers start with their conclusions and work backwards to retrofit the "evidence." Doctors who do the same shouldn't be regarded any differently.

Steve Kirsch and Brandolini’s law
The amount of energy needed to refute bullshit is an order of magnitude bigger than that needed to produce it.

