Legislative Alchemy 2017: Acupuncture
Acupuncture is nothing more than a theatrical placebo. Yet acupuncturists, defined as primary care practitioners in some states, are succeeding in licensing and practice expansion efforts in state legislatures.
Cancer quack Colleen Huber sues Britt Hermes over criticism
Naturopathic cancer quack Colleen Huber is attempting to silence criticism of her practices by suing Britt Hermes. Help Britt fight back with a donation to help defray legal expenses.

The Elephant in the Compounding Pharmacy
Contaminated products from compounding pharmacies have harmed and even killed patients. Quality control measures are being implemented, but there is a bigger problem: the injudicious use of untested and potentially dangerous treatments.

The final push to pass a federal version of the cruel sham of “right-to-try” is under way
Right-to-try laws are a cruel sham that claim to help terminally ill patients by providing them with earlier access to experimental therapeutics, even though they do very little in this regard. Promoted primarily by the libertarian think tank the Goldwater Institute, in reality they are a strategy to weaken the FDA's regulatory power to assure that marketed drugs are safe and effective....

Legionnaires’ Disease: The Other Disneyland Outbreak
As 2017 came to a close, Disneyland again played a role in the outbreak of an infectious disease, this one much more deadly than measles.

Medical Marijuana: Where is the evidence?
Marijuana is widely touted as an effective medicine for an array of conditions. But what does the evidence actually tell us?
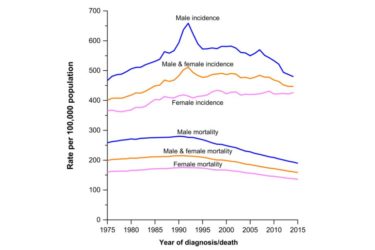
Cancer Deaths Continue to Decline
Overall cancer incidence has been stable in women and declining steadily in men. Changes in specific cancers reflect known risk factors and the effect of screening methods. What is not seen in this data is any mysterious increase in any specific cancer or cancers overall.
Five Fatal Foods
Dr. Nina Koduru identifies 5 fatal foods that endanger your life and offers a solution: an untested remedy with unsubstantiated claims.






Infiltrative Pseudoscience
If you don't think that CAM is the enemy of science in medicine, then you don't understand CAM and its proponents. Don't be fooled by their marketing. They want a return to the pre-scientific days when health gurus could sell any snake oil they want at exorbitant prices, with any hyped claims that they want, without going through all that tedious science.