Science-Based Satire: Australian Fetus First to Undergo Intrauterine Chiropractic Adjustment
Are chiropractic surgeons really performing intrauterine spinal adjustments based on the results of nonsensical muscle tests and ultrasound imaging? No.

Is something better than nothing? The many ineffective ways we treat nocturnal leg cramps
While leg cramps won't kill you, they can make you miserable when you are trying to sleep. There's not much evidence for effective treatments, and there are far more proposed treatments than there is evidence.

Video Games and the Brain
A new article looked at the effect of playing video games on the brain. Its results confirm what was previously suspected from prior research. First, it is another demonstration of use-dependent plasticity in the brain. Further, it supports a direct relationship between the types of activity in which people engage and increases or decreases in the respective parts of the brain. And...

Doc Doc Zeus: A Glimpse Behind the Scenes of Medical Boards
A novel about a doctor who raped a minor and is being investigated by his state medical board provides behind-the-scene insights into the workings of medical boards. It helps explain why these boards are so often ineffective, why medical malfeasance so often leads to a token disciplinary action rather than to loss of license.

Naturopathy and dubious compounding pharmacies: A deadly combination
In March, it was widely reported that a young woman named Jade Erick had died suddenly of a hypersensitivity reaction while undergoing an infusion of intravenous curcumin ordered by a naturopath named Kim Kelly to treat her eczema. The FDA investigated and found egregious problems with the injectable curcumin used. This tragic incident thus serves to demonstrate how dangerous a combination naturopaths...

The cruel sham of “right-to-try” takes a giant step towards becoming federal law
So-called “right-to-try” is a cruel sham that holds out the false hope of survival to terminally ill patients and their families. In return, all they have to give up is patient protections and agree to pay to be guinea pigs to test a drug company’s product. The product of an ideology that uses the terminally ill as shields to hide the ideological...

Integrative Psychiatry
Alternative medicine is not just restricted to physical health. Practitioners have insinuated themselves into mental health as well, to the detriment of patients and science.
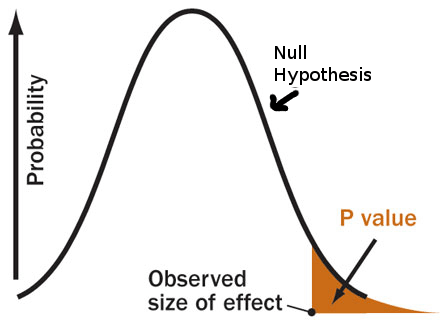
0.05 or 0.005? P-value Wars Continue
The p-value is under fire yet again, but this time with some quick-and-dirty solutions (and some long-and-onerous ones too) to the problems created by relying on this quick-and-dirty test.

The Antithesis of Science-Based Medicine: The Medical Medium’s Fantasy-Based Health Advice
Anthony William, the Medical Medium, hears voices that give him advanced scientific information from the spirit world. He offers reams of health advice based on nothing but fantasy. He even tells readers to call on 12 angels out loud by their name. I call bull.