
So Long and Thanks for All the SCAM
So long/Farewell/Auf wiedersehen/Adu/Adu adu to you and you and you.

“Chronic Lyme” VIP Daniel Cameron disciplined by New York medical authorities
"Chronic Lyme" guru Daniel Cameron, MD, has been put on 3-year probation by New York medical authorities. Will fellow "Lyme literate" doctors take note?

Coconut Oil Warning
Coconut oil is promoted as a health food, but a recent warning from the American Heart Association warns that coconut oil is very high in saturated fats and increases your risk for heart disease.

Fun with Spanish Flu Myths
There are many myths about the Spanish flu pandemic of 1918. Some of them are pretty funny.

The sad but unexpectedly hopeful cancer saga of Cassandra Callender
I've frequently discussed the stories of teenagers with cancer who either refuse chemotherapy or whose parents refuse chemotherapy for them. The case of Cassandra Callender is the same, yet different, from many of these unfortunate and sad sagas in that she was older when diagnosed with cancer and that she realized her mistake. I can now only hope that it's not too...

The Ethics of Involuntary Pediatric Drug Testing
Although it may seem like a good idea, testing for recreational drug use on an adolescent patient without consent is ethically questionable, challenging to interpret, and unlikely to benefit patient or family.
A closer look at penicillin allergies
While many people believe they may be allergic to penicillin, few actually are. The consequences may be serious.
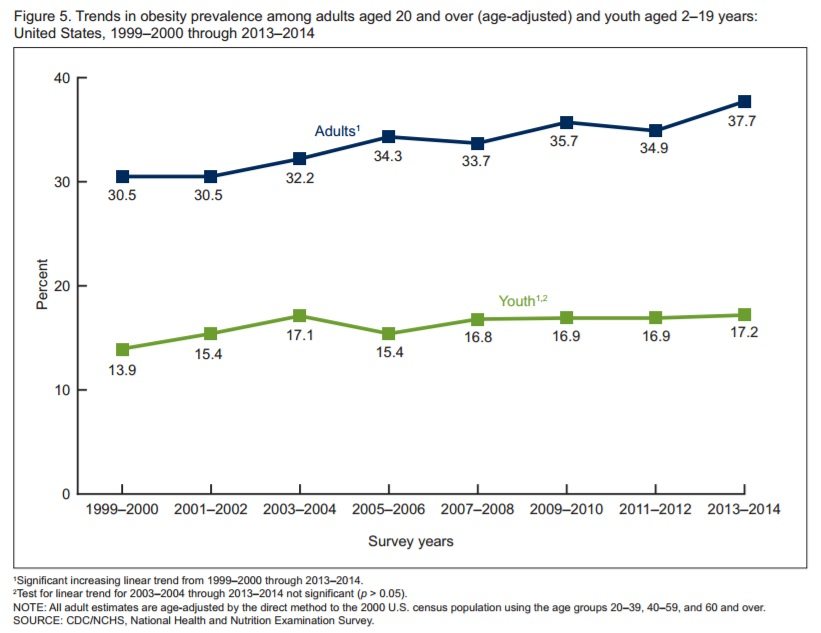
BMI and the Obesity Epidemic
Obesity is a serious and growing health problem worldwide. Ditching BMI as a measure of obesity is not the solution.

On Guard, DōTERRA, Essential Oils, and a Lesson in Reading Research Studies
A study of On Guard™, a mixture of essential oils, showed that it reduced the infectivity of influenza virus in dog kidney cells in the lab; but that's irrelevant to the question of whether the product has any clinical effect in humans.

Does society try to shame and shun vaccine refusers and the vaccine-averse?
Antivaxers often complain that they are judged harshly, even shunned. A recent study suggests that, to some extent, they might well be. But are judging, shaming, and shunning parents who refuse to vaccinate their children wrong? More importantly, what about the children, who didn’t choose not to be vaccinated, and how likely is such stigmatization to change behavior?






Don’t Blame the Patient