The Ethics of Artificial Brains
We are living in a time of technology advancing so rapidly it is challenging to keep up. This has multiple ramifications, and in the area of biomedical research, there is an important ethical and regulatory dimension. Confronting the ethical considerations of our own technology is nothing new, and fresh debate seems to erupt with every new development – including in-vitro fertilization, transplanting...
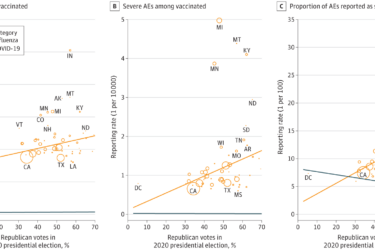
Dr. Vinay Prasad vs. a VAERS study finding more reports of vaccine injury in red states
Dr. Vinay Prasad attacks an epidemiological study published in JAMA Open Network reporting that people in red states are more likely to report vaccine injuries, claiming that a more rigorous study would "not be difficult," when he knows that it would be very difficult.

Every Time Dr. Jay Bhattacharya Talks About COVID, He Proves He Was Totally Wrong About COVID
Dr. Jay Bhattacharya March 2020: "If it’s true that the novel coronavirus would kill millions without shelter-in-place orders and quarantines, then the extraordinary measures being carried out in cities and states around the country are surely justified."

Skeptics in the Pub. Cholera. Chapter 15 minus 1
For those more observant than a semi-senile old man, I cut and pasted the wrong text this morning. Now updated. Good thing I am retired.

The Failed “We Want Them Infected” Movement Is Trying to Rebrand Itself As The “All We Really Wanted Was Poor Kids in School” Movement.
Part 2: In 2020, pro-infection doctors said "It’s fantastic news that we have a lot of cases." Today, they performatively lament "learning loss for children, especially in poor families". What happened to their assurances that the mass infection of unvaccinated youth will rapidly lead to herd immunity?
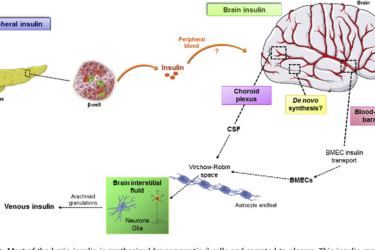
What Is Type 3 Diabetes?
I’m always wary of new medical terms that seem to be used and promoted prematurely, when still in the hypothesis phase. It seems like an obvious way to bias any thinking about an alleged phenomenon – just label it as the hypothesis, as if it is already a conclusion. Calling symptoms that may follow a lyme infection “chronic lyme disease” implies something...

The Truth vs. Alex Jones: How the DSHEA of 1994 gave conspiracy mongers the means to fund their empires
As the HBO documentary The Truth vs. Alex Jones shows, Alex Jones promoted the conspiracy theory that the Sandy Hook massacre was a hoax to sell his supplement line. It's a model that many Internet conspiracy theorists use, like Mike Adams. Did the DSHEA help create Alex Jones and the modern conspiracy industry?

Dr. Marty Makary: “We’ll Have Herd Immunity by April” & “It’s Okay To Have an Incorrect Scientific Hypothesis. But When New Data Proves It Wrong, You Have To Adapt.”
Part 1: Doctors who said the pandemic ended 3-years ago now have the audacity to lament the "damaged public trust in the medical profession."

Skeptics in the Pub. Cholera. Chapter 13
Saturday. Just another workday when the Cholera is flowing. I woke early, at 6 a.m., and went to the office before anyone else. On the way, I went to the grocer’s and bought some supplies. I started, as usual, in the cubby room, and I was happy to see that as of yesterday that cases of the Cholera were staying down: there were...
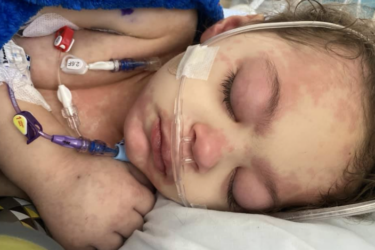
COVID-19 Vaccination Significantly Reduces Risk of Severe Inflammatory Syndrome in Kids
A new analysis of 2023 MIS-C cases reveals that the COVID-19 vaccine significantly reduces the risk of this dreaded complication.





