Tag: stroke

A Poorly Conceived Study Fails to Prove Ayurveda Works
Quackery is alive, well, and government-supported in India, as demonstrated by a terrible study of Ayurveda.
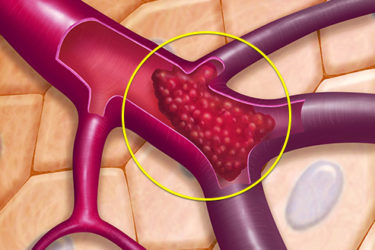
Stroke in COVID-19 Patients
A case series of five patients with COVID-19 and young strokes sparks many questions.
Another serious complication from chiropractic cervical manipulation: Vertebral fracture leading to paralysis and death
John Lawlor was an 80 year old man with leg pain. Thinking he was going for physiotherapy, he ended up in the office of Arleen Scholten, a chiropractor. What happened next involved cervical spine manipulation, vertebral fracture, death, and a lack of accountability.

The adverse health effects of the lunacy that is Daylight Saving Time
Daylight Saving Time has been around for over 100 years. Why does it still persist when there's little or no evidence that it does what it was intended to do (save energy) and growing evidence of adverse health effects related to the twice a year time change? That's a good question. It's time to get rid of this antiquated practice.

The stem cell hard sell, Stemedica edition
Stemedica Cell Technologies, a San Diego company that markets stem cell treatments for all manner of ailments, likes to represent itself as very much science-based. There are very good reasons to question that characterization, based on the histories of the people who run the company, as well as the company's behavior.
Carotid Artery Stenosis: Surgery, Stent, or Nonsurgical Stroke Prevention?
The carotid artery in the neck is a common site of atherosclerosis. As plaque builds up, it leaves less room for blood flow and can cause strokes through clotting or embolization. Carotid stenosis is defined as a greater than 70% narrowing of the lumen (the space through which the blood flows in an artery). It can cause symptoms, including transient ischemic attacks...

Did chiropractic neck manipulation kill Katie May?
Well, we’re back. Yes, after having our WordPress database somehow borked to the point where no new posts could be added and no existing posts could be edited since Friday, Science-Based Medicine is back in business—finally! As a result, some of you might have seen this post elsewhere, as it was considered to be somewhat time-sensitive, and I didn’t want to delay,...

Stem cells versus Gordie Howe’s stroke, part 3
Here I am in Philadelphia attending the 2015 American Association for Cancer Research (AACR) meeting to imbibe the latest basic and translational science about oncology. So what am I doing in my non-conference time? I’m holed up in my hotel room near Rittenhouse Square writing a DoD Grant and this post. Fortunately, I am nearly done with the grant, with nothing I...

An aboriginal girl dies of leukemia: Parental “rights” versus the right of a child to medical care
One topic that keeps recurring and obligating me to write about it consists of critically analyzing stories of children with cancer whose parents, either on their own or at the behest of their child, stop or refuse chemotherapy or other treatment. It is, sadly, a topic that I’ve been discussing for nearly a decade now, starting first on my not-so-super-secret other blog...


