Category: Basic Science
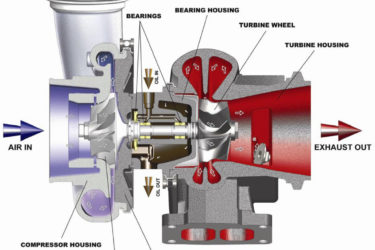
COVID-19 vaccine-caused “turbo cancer” nonsense just keeps getting more turbocharged
No matter how implausible it is or how weak the evidence for it is, the myth that COVID vaccines cause "turbo cancer" just won't die. Quite the contrary, alas. Antivaxxers are—dare I say?—turbocharging it with bad science.

Antivax quacks are continuing to make up fantastical biological mechanisms for COVID-19 vaccine “shedding”
A couple of weeks ago, I discussed why antivax quacks' claimed biological mechanisms for COVID-19 vaccine "shedding" reminded me of homeopaths. Confabulation about fantastical scientific mechanisms continues, courtesy of "A Midwestern Doctor."
“New school” antivax goes old school as Byram Bridle asks if COVID-19 vaccines will drive an “epidemic” of autism
Wakefield redux? Antivax scientist Byram Bridle just took the "new school" antivax movement old school by implying that COVID-19 vaccines might cause an "epidemic of autism." Everything old is new again, sort of.
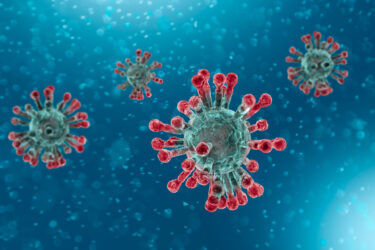
Why antivax arguments for COVID-19 vaccine “shedding” remind me of homeopathy
An antivaxxer by the 'nym "A Midwestern Doctor" makes an argument that COVID-19 vaccine "shedding" is not impossible despite the basic science that concludes it is. Sound familiar?
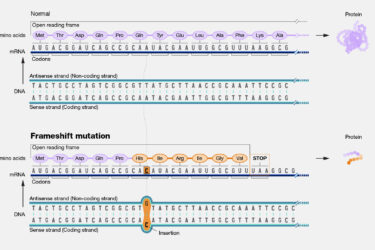
Do mRNA vaccines produce harmful “junk proteins” that “gunk up” the cell and cause unintended “off-target” immune responses?
A new study is making the rounds in the antivax crankosphere. The study found that the modified mRNA used in the Pfizer vaccine can cause a frame shift (to be explained) that results in the production of proteins besides the intended spike protein. The findings are, as you probably guessed, a big nothingburger compared to how they are being spun.
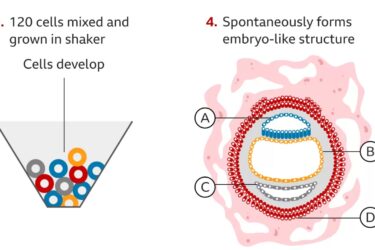
Complete Human Embryo Model Made From Stem Cells
Researchers create an embryo model from human embryonic stem cells.
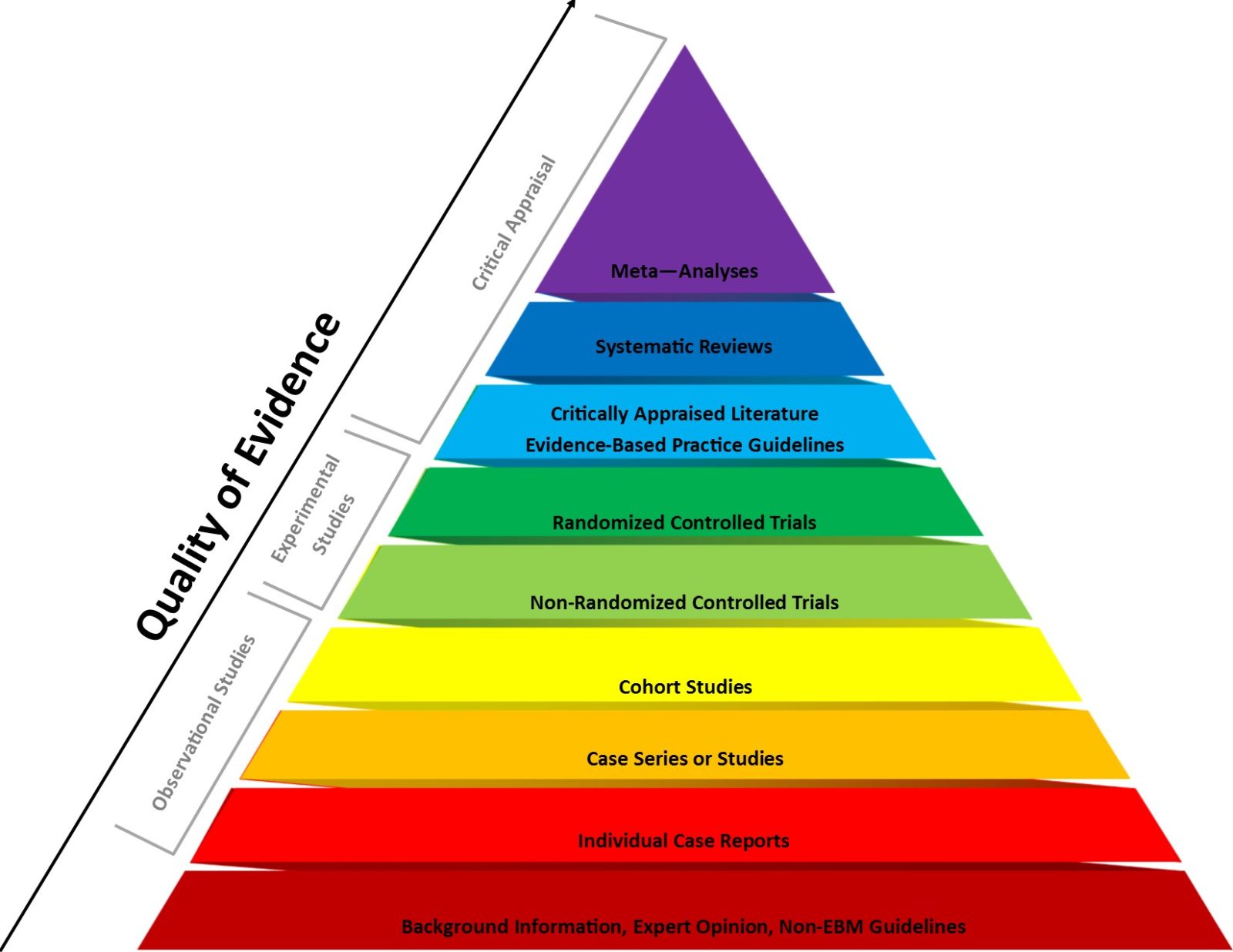
Evidence-based medicine vs. basic science in medical school
Last week Dr. Vinay Prasad wrote a Substack arguing that medical students should learn the principles of evidence-based medicine before basic science.This is a recipe for amplifying the main flaw in EBM that science-based medicine was meant to correct, and Dr. Prasad's arguments would have been right at home on an integrative medicine blog. [Note ADDENDUM.]

Part of a Complete Breakfast
Infection control. When one adheres to compliance it is effective. Like masks and COVID 45.

After 15 years of SBM: Lessons learned and what the future holds
Last week, Dr. Novella discussed what SBM has accomplished over the last 15 years. I'm going to discuss lessons learned, what has changed, and remaining huge challenges. Unfortunately, after the pandemic, our position in 2022 reminds me even more than ever of Aragorn at the Black Gate of Mordor, but that does not mean things are hopeless.


Madonna !?!
Remembering the old days of Madonna, courting, and naloxone use.