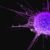
Dr. John Ioannidis: “The Biggest Mistakes I am Sure Are Mine.”
Part 3: Dr. John Ioannidis said his biggest mistake was the he "underestimated how much power politics and media and powers outside of science, could have on science." Really?

UK’s Phased Smoking Ban
UK MPs have just passed the Tobacco and Vapes Bill by a 383 to 67 vote. If the measure becomes law it will ban the sale of tobacco products to anyone born after January 1, 2009. This is not just an age limit – this is a permanent phased ban. If the law passes and stands, anyone born after that date will...

Tongue
TCPM Tongue diagnosis. Garbage in, garbage out.
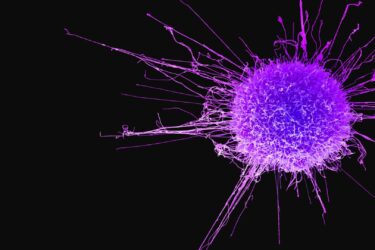
There is no evidence that COVID-19 vaccines are causing cancers associated with “accelerated aging”
A recent presentation at AACR found a link between markers of accelerated aging and an increased risk of cancer. Then antivaxxers got a hold of it to blame COVID-19 vaccines not just for cancer, but for "accelerated aging" causing it.

Dr. Vinay Prasad: It’s “Good” That Parents Who Want To Vaccinate Their Kids Against COVID Get Reported To Child Protective Services
Trying to limit pediatric COVID was literally the pandemic's worst sin for pro-infection doctors, warranting severe punishment. This is how desperately they wanted them infected.

Skeptics in the Pub. Cholera. Epilogue
I felt remarkably well when I awoke despite the previous night’s beer. I was a little thirsty, and my mouth felt like I brushed my teeth with a toilet brush. I took a long shower and took my time getting ready for work. I bought a scone and tea on my way to the trolley and picked up a newspaper. For the...

New Study Finds No Link Between Autism and Acetaminophen Use During Pregnancy
A new study designed to better account for hidden confounding factors has found no link between acetaminophen use during pregnancy and the risk of neurodevelopmental conditions in childhood.

SARMs Harms
Selective androgen receptor (SARMs) are sports supplements marketed to teens via social media influencers.
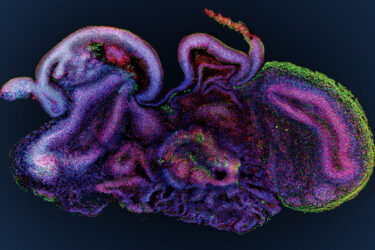
The Ethics of Artificial Brains
We are living in a time of technology advancing so rapidly it is challenging to keep up. This has multiple ramifications, and in the area of biomedical research, there is an important ethical and regulatory dimension. Confronting the ethical considerations of our own technology is nothing new, and fresh debate seems to erupt with every new development – including in-vitro fertilization, transplanting...
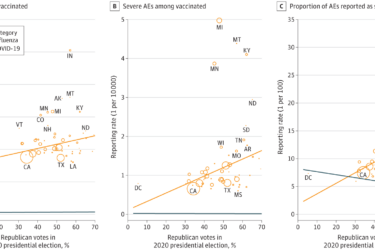
Dr. Vinay Prasad vs. a VAERS study finding more reports of vaccine injury in red states
Dr. Vinay Prasad attacks an epidemiological study published in JAMA Open Network reporting that people in red states are more likely to report vaccine injuries, claiming that a more rigorous study would "not be difficult," when he knows that it would be very difficult.