
U.S. Infant Mortality Increases for First Time in 20 Years
Recently published CDC data has revealed an increase in the number of infant deaths in 2022, the first in two decades. The United States continues to struggle with serious healthcare disparities and to lag behind other countries when it comes to keeping young children alive.

Science-Based Satire: Chiropractors Brace for November Neck Pain Tsunami
Are men who grow a beard next month at risk of neck injuries caused by chiropractic subluxations? Of course they are. And what about those leftover pandemic beards? Shave. Shave now! This is definitely a real problem. I mean, I can't just make something up...on the internet.

Hitting Children in School: Bad?
The title of this post is silly. Hitting kids in school is always bad, and there is very good reason to expect the same negative outcomes from school-based corporal punishment as are seen when kids are hit at home. The AAP recently recently released a policy statement calling for a national ban.

A Nice Chat with The Infant Feeding Alliance on Breastfeeding Promotion Pitfalls
Last week I had the pleasure of sitting down with Ruth Harpur from the Infant Feeding Alliance for a nice chat about problems with aggressive breastfeeding promotion.

Did a Spicy Social Media Challenge Kill a Massachusetts Teen?
Did an absurdly spicy chip and a social media challenge kill a Massachusetts teen? His family sure thinks so, and it is possible. But skepticism is appropriate unless further details emerge. Still, these chips aren't for kids.
Science-Based Satire: TCM Experts Baffled by Man Born Without Meridians
Has the first case of complete congenital Qi deficiency been diagnosed in Massachusetts? Is it possible to run a successful landscaping business without any meridians? Where can you get acupuncture and your car detailed at the same time? All these questions and more will be answered in today's post, which I completely made up.
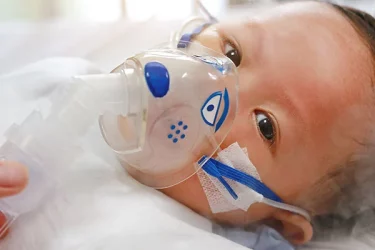
Nirsevimab is Great News for Infants, Caregivers, and Exhausted Pediatricians
RSV is a terrible infection that puts thousands of kids in the hospital every year and can be deadly. We will soon have a safe and effective way to prevent many of these severe cases, but it won't be easy to get shots into arms this season.

Should Protein Powder Have a Warning Label?
The unfortunate death of a teen in London has some experts calling for new warning labels on products containing large amounts of protein. But would that work?
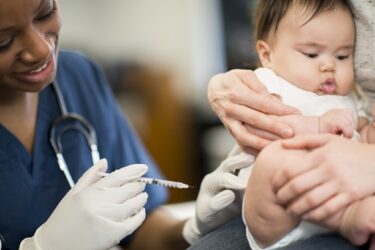
Childhood Vaccination Rates Move (Slowly) in the Right Direction
Childhood vaccination rates worldwide tanked during the first two years of the pandemic. A recently released report from the UN revealed that 2022 was better, but the improvements weren't seen everywhere. And we still have a long way to go.

Delabeling Penicillin Allergies: A Public Service Announcement from Science-Based Medicine
Is your child allergic to penicillin? Are you sure about that? Penicillin allergy is much less common than widely believed and there is a big push to delabel pediatric and adult patients who actually can tolerate these antibiotics.

