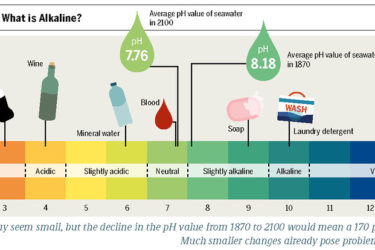
Skin pH: Salesmanship, Not Science
People are being encouraged to worry about the pH of their skin and to try to change it. These concerns and interventions are not supported by scientific evidence.

New Drug Is Effective for Post-Partum Depression, But There Are Drawbacks
A new drug promises to cure postpartum depression, but it is restricted and patients must be hospitalized for a 60-hour IV infusion.

Can A One-Minute Cure Really Heal Virtually All Diseases?
The author of this book claims to have found a one-minute cure that will heal virtually all diseases. The claim is ludicrous, and is not supported by any evidence.

Juice Plus+: Good Marketing, Not Good Science
Juice Plus+ is a multilevel marketing company selling fruits and vegetables that they have reduced to a powder and put into capsules. It's clever marketing using deceptive advertising. There is no scientific evidence that it benefits health.

Treating Mental Illness with Nutrition: The Walsh Protocol
The Walsh Institute offers the Walsh protocol for the nutritional treatment of mental illness. This "orthomolecular psychiatry" is not supported by any clinical studies.

The Best Science from The New England Journal of Medicine
The editor-in-chief of The New England Journal of Medicine has selected a dozen articles published during his tenure that epitomize the best of science-based medicine.
SmartJane Test of Vaginal Health: Clever Marketing, Questionable Science
uBiome claims that its SmartJane test's proprietary technology empowers customers to assess their own vaginal health. The company is being investigated for fraudulent billing practices, and the rationale for the test makes no sense.

The Scientific Attitude, Not the Scientific Method, Is the Key
A philosopher of science argues that science is not characterized by a specific scientific method but by the scientific attitude. Scientists value empirical evidence and follow the evidence wherever it leads. They are open to changing their mind rather than stubbornly clinging to an ideological belief system.

Pseudoscience in Child and Adolescent Psychotherapy
This new book addresses the neglected field of research on child and adolescent psychotherapy and does an excellent job of distinguishing treatments that have been proven to work from treatments that are based on pseudoscience.


