New CMS Chief Donald Berwick: a Trojan Horse for Quackery?
NB: I posted this on Health Care Renewal a couple of days ago, figuring that Dr. Gorski’s post would suffice for the SBM readership (he and I had discussed the topic while at TAM8 last week). But Managing Editor Gorski has asked me to repost it here, which I’m happy to do. I am especially pleased to demonstrate that I am capable...
Doctor’s Data Sues Quackwatch
A few weeks ago I posted an article about bogus diagnostic tests. I cited Doctor’s Data, Inc. (DDI), as “a company with a long history of dubious offerings.” I also wrote: You can’t help but have noticed that many of the links in this post are to articles on Quackwatch. That’s because the site is chock full of useful information about bogus tests,...
Professional Integrity for Sale? “Sure,” Says Medscape!
Some chiropractors also practice homeopathy. According to Frank King, D.C., many more should be doing just that: Homeopathy is an energetic form of natural medicine that corrects nerve interferences, absent nerve reflexes, and pathological nerve response patterns that the chiropractic adjustment alone does not correct. The appropriate homeopathic remedies will eliminate aberrant nerve reflexes and pathological nerve responses which cause recurrent subluxation...
The Weekly Waluation of the Weasel Words of Woo #10
The W^5/2 Hits Double Figyiz! OK, I gotta admit that my friend Orac moved me to render this Special 10th Edition of the W^5/2™ (after a brief hiatus) by mentioning it today in the context of an article that used, er, the topic of our venerable game to great advantage! Some of it is brilliant, unprecedented even: Perhaps most tellingly, the U.S....
Bogus Diagnostic Tests
A few years ago a friend asked me to comment on advice given to her adult daughter by a psychiatrist whom she’d consulted for depression. The psychiatrist had recommended testing samples of saliva and urine for hormone and neurotransmitter levels, the results of which would likely indicate a need for supplements to correct deficiencies or imbalances. According to the psychiatrist, who had...
My NCCAM Wish List
For a number of reasons, well-argued many times here on SBM, it would be beneficial to American citizens if the National Center for Complementary and Alternative Medicine (NCCAM) were abolished. This does not seem to be in the cards anytime soon. Here, then, are my suggestions for making the Center less dangerous and less of a marketing tool for pseudomedicine than it...
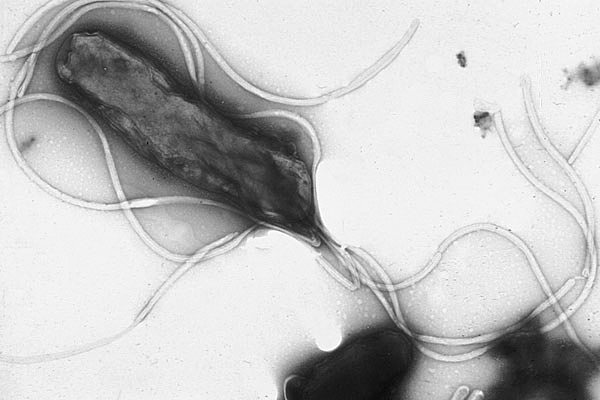
H. Pylori, Plausibility, and Greek Tragedy: the Quirky Case of Dr. John Lykoudis
Mark Crislip is on vacation, but through an arduous series of shakings and succussions (beating his head against the wall?) we have channeled part of his essence: This post mostly concerns itself with infectious diseases, thanks to several recent posts on SBM that discussed the plausibility of health claims† and that touched on the recent discovery that most peptic ulcer disease (PUD)...
KA at Boston Skeptics in the Pub March 29
Yers truly will speak at Tommy Doyle’s, Harvard Square, Cambridge. 7:00 PM on March 29. Title: Implausible Health Claims and Human Studies Ethics: A Collision Course Description: A broad international consensus regarding protections for subjects in human trials emerged during the 2nd half of the 20th century. It can be summarized in several tenets, most of which pertain explicitly or implicitly to scientific...
The 2nd Yale Research Symposium on Complementary and Integrative Medicine. Part II
The Main Event: Novella vs. Katz The remainder of the Symposium comprised two panels. The first was what I had come to see: a Moderated Discussion on Evidence and Plausibility in the Context of CAM Research and Clinical Practice, featuring our Founder, Steve Novella, who is also Assistant Professor of Neurology at Yale; and David Katz, the speaker who had borne the...
The 2nd Yale Research Symposium on Complementary and Integrative Medicine. Part I
March 4, 2010 Today I went to the one-day, 2nd Yale Research Symposium on Complementary and Integrative Medicine. Many of you will recall that the first version of this conference occurred in April, 2008. According to Yale’s Continuing Medical Education website, the first conference “featured presentations from experts in CAM/IM from Yale and other leading medical institutions and drew national and international...

