Heart disease: one of science-based medicine’s great successes
Sixty years ago, the world was full of miracles. Western Europe was recovering from the devastation of World War II, an agricultural revolution promised to banish the fear of starvation in large parts of the world, and the mythical Mad Men era gave Americans a taste of technology-dependent peace and prosperity unlike any in the past. Despite the technological progress that would...
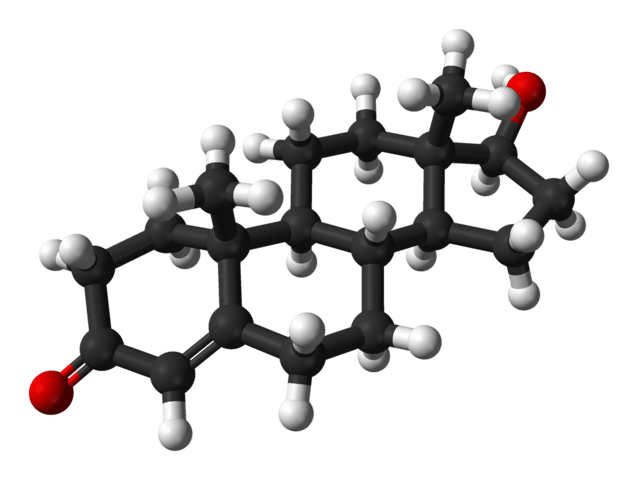
Do you have low T?
Testosterone replacement - panacea, or snake oil? Of course, it's not that simple.
Christiane Northrup: more bad medicine
A question popped up on facebook the other day about Dr. Christiane Northrup, an OB/GYN who has been a frequent guest on Oprah. I hadn’t heard much about her for a while, but a foul taste still lingered from previous encounters with her work. So I went over to her website to see what fare she’s currently dishing up. It isn’t pretty....
Your disease, your fault
Earlier this week, my colleague Dr. Gorski explored a common theme in alternative medicine: the idea that all disease is preventable. This implies that all disease has a discrete cause and that individual behavior can mitigate this cause. If biology worked this way, my job as an internist would be very different. Many people would love to believe that life is this...
Why bother?
It can be rather frustrating to refute the same old canards about alternative medicine. There’s always been argument as to whether this is even useful. Critics (some verging on “concern troll-ism”) argue that skeptics are convincing no one, others that we are too “dickish”. The first view is overly pessimistic (re: our impact), the second overly optimistic (re: the benign nature of...
Homeoprophylaxis: An idea whose time has come—and gone
One of the strengths of modern medical education is its emphasis on basic science. Conversely, the basic weakness of so-called alternative medicine is its profound ignorance of science and its reliance on magical thinking. Nowhere is this more apparent than in the attempts of altmed cults to conduct and publish research. From “quantum water memory” to “almost as good as placebo”, the...
HuffPo blogger claims skin cancer is conspiracy
I was a bit torn when trying to figure out how to approach this piece. A reader emailed me about an article in the Huffington Post, and there is so much wrong with it that I felt overwhelmed. My solution is to focus on a few of the problems that can help illuminate broader points. There is a small but vocal movement...
It sounds so “nutritionous”
Dietitians are a critical part of modern medicine. In the hospital, dieticians not only educate patients on dietary treatment of diseases such as diabetes and heart disease; they also evaluate the nutritional status of critically ill patients and develop nutrition plans that may involve tube feeding or intravenous feeding. This is complicated, and takes into account a patient’s nutritional needs, medical conditions,...
Narcotic treatment contracts and the state of the evidence
Opium derivatives—and later, synthetic opioids—have probably been used for millennia for the relief of pain. Given human biology, they’ve probably been abused for just as long. Opiate use disorders are a daily fact for primary care physicians; the use of these drugs has become more and more common for chronic non-cancer pain. These medications are very effective in the treatment of pain,...
Naturopathy for allergies
Naturopathy is an unusual chimera. It is basically a collection of old fashioned medical superstitions presented under a veneer of highly speculative, quasi-scientific assertions. But given its popularity, it is important, from time to time, to evaluate specific claims made by this particular non-science-based belief system. A reader informed me that he was advised to seek the advice of a naturopath for...

