Chiropractic and Spinal Manipulation Red Flags: A Comprehensive Review
Many people visit chiropractors’ offices seeking relief from back pain. Appropriate use of spinal manipulation provided by a chiropractor can be helpful in treating mechanical-type back pain, but there are good reasons to avoid chiropractic manipulation based on correction of “vertebral subluxations,” and there are red flags to look for before undergoing any kind of manipulative treatment for neck or back pain.
Chiropractic Subluxation Theory: Legal Support for Inappropriate Use of Spinal Manipulation
Legally licensed, unbridled subluxation-based chiropractors who offer unproven treatment for a broad scope of health problems endanger public health, stigmatize appropriate use of spinal manipulation, and deter development of chiropractic as a legitimate back-care specialty.
Cervicogenic Headache and Cervical Spine Manipulation
NOTE: Today we offer a double feature on the treatment of cervicogenic headache: this post and Dr. Harriet Hall’s post, “When Headaches Are a Pain in the Neck: Spinal Manipulation vs. Mobilization for Cervicogenic Headache.” They complement each other, as well as Dr. Hall’s post from last week on the possible risk of stroke with neck manipulation. A cervicogenic headache has been...
Subluxation Correction: A Chiropractic Treatment for Babies
My article “Pediatric Chiropractic Care: The Subluxation Question and Referral Risk” was published in the 2016 February issue of the journal Bioethics. The abstract summarizes the message of the article: Chiropractors commonly treat children for a variety of ailments by manipulating the spine to correct a “vertebral subluxation” or a “vertebral subluxation complex” alleged to be a cause of disease. Such treatment...
The Enigma of Chiropractic: A Brief Review with a Perspective on Chiropractic as a Specialty
Much of what is discussed in this article has been said before in previous articles I have written for Science-Based Medicine. But since the audience for SBM has greatly increased over the past few years, some subject matter should be repeated for the new readers and researchers coming to this site for reliable information on health care. Many consumers now search SBM...
Opposing Chiropractic: Persecution or Justified Criticism?
The saga of chiropractic began in 1895 when D.D. Palmer, a magnetic healer, announced that “95 percent of all diseases are caused by displaced vertebrae, the remainder by luxations of other joints.” Palmer opened the first chiropractic school in Davenport, Iowa, offering a three-week course of study at the Palmer School and Cure, subsequently renamed the Palmer School of Chiropractic. The school...
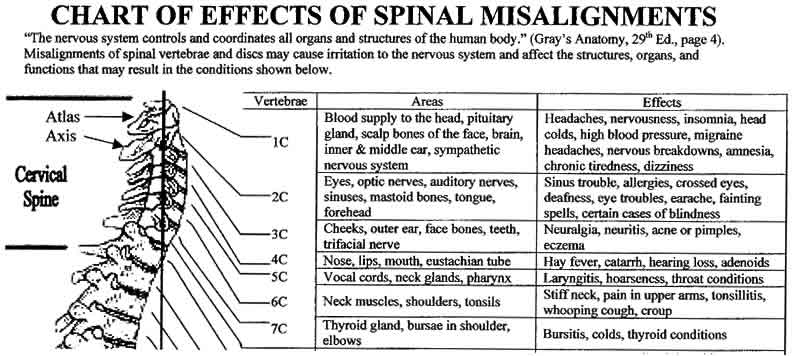
Questions and Answers about Chiropractic: The Bottom Line
I am often asked, “What do chiropractors do?” That’s not an easy question to answer. The answer is usually expected to be, “They treat back trouble.” But as alternative medicine practitioners, chiropractors do a lot of things, and they treat a variety of ailments, based largely on a scientifically-invalid vertebral subluxation theory which proposes that nerve interference resulting from a misaligned vertebra...
Upper Neck Manipulation: Caveats for Patients and Providers
Chiropractors often deny that neck manipulation can be a primary cause of stroke by injuring vertebral arteries. But according to Jean-Yves Maigne, M.D., head of the Department of Physical Medicine at the Hôtel-Dieu Hospital in Paris, France: It is now a well established fact that cervical thrust manipulation can harm the vertebral artery. This accident was formerly regarded as very rare, although...
Chiropractic Defense: Tempest in a Teapot
When Forbes.com published Steven Salzberg’s article “New Medicare Data Reveal Startling $496 million wasted on Chiropractors” (April 20, 2014), a flood of mail (more than 300 comments) from chiropractors and their patients provided a wealth of evidence that subluxation-based chiropractic is alive and well despite rejection by the scientific community. Pro-chiropractic comments laced with anti-medical rhetoric and ad hominem attacks, expressed with...