
Keto Diet for Neurological Disorders
Does the ketogenic diet work for epilepsy or other neurological disorders? While the consensus is that it probably does, the evidence is surprisingly thin.
The Myth of Vaccine Shedding
No - the measles vaccine cannot cause an outbreak through virus shedding, but this myth persists in antivaccine circles.

Psychological Placebos
New research shows the importance of carefully separating real therapeutic effects from psychological placebos.
Is An Israeli Company About to Cure Cancer?
Hyped claims for a cure for all cancers are inherently unbelievable. So don't believe them.

WHO – Vaccine Hesitancy Top Health Threat
The World Health Organization recognizes that vaccine-hesitancy is a top threat to the public health. Now what are they going to do about it?

Frequency Specific Microcurrent
Frequency Specific Microcurrents is a dubious energy medicine treatment in the tradition of Albert Abrams.
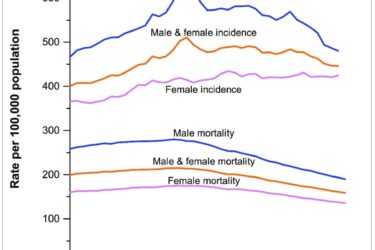
Cancer Death Rate Continues to Decline
The new data are in – cancer deaths continue to decline at a steady rate.
Regulating Fringe Practitioners
Fringe professions like chiropractic and naturopaths are not adequately regulated. This needs to be fixed.

Release Active Drugs – Homeopathy By Another Name
A Russian company is marketing "release active drugs" as a new medical technology, but it is just bogus homeopathy dressed up with new jargon.


SBM in 2018 and Beyond
A look back at SBM in 2018 and the future of SBM.