
Quackademic Medicine at UC Irvine
UC Irvine Medicine School opens a center for integrative medicine, selling out to promote quackery in medicine.

Faith and Supplements – B17
Amygdalin is a toxic snake oil dating back to 1830, but it is still sold today with a combination of supplement industry deception, faith, and conspiracy theories.
Naturopathic Cancer Quackery
Naturopaths treat cancer with an array of implausible concoctions that are not based on clinical science, and then defend themselves with cease and desist letters.

Panera Markets Food Fear
Panera Bread goes full Food Babe in their latest ad campaign, which fearmongers about a safe food preservative.
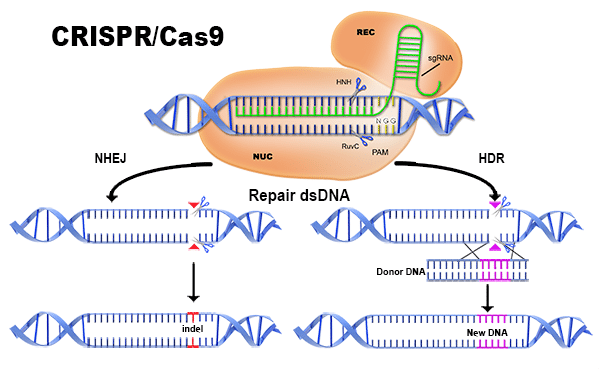
The Promise of CRISPR
CRISPR is the latest rock-star medical technology that promises to revolutionize medicine. Let's take a look at the hype and the reality.

The Supplement Con
A new article in Business Insider challenges the major narrative promoted by the supplement industry - that supplements are safe, effective, natural, and actually in the bottle. If we are lucky, this may mark a the start of a sea change in how Americans see supplements.

Video Games and the Brain
A new article looked at the effect of playing video games on the brain. Its results confirm what was previously suspected from prior research. First, it is another demonstration of use-dependent plasticity in the brain. Further, it supports a direct relationship between the types of activity in which people engage and increases or decreases in the respective parts of the brain. And...
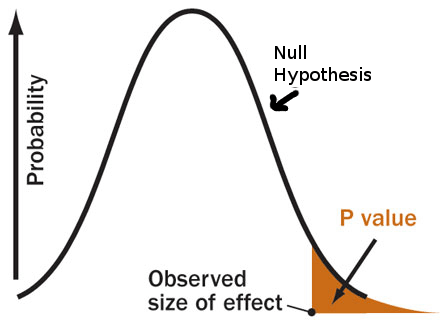
0.05 or 0.005? P-value Wars Continue
The p-value is under fire yet again, but this time with some quick-and-dirty solutions (and some long-and-onerous ones too) to the problems created by relying on this quick-and-dirty test.

Increase In Supplement Poisonings
Current supplement regulations in the US (and many countries) are overtly anti-consumer and pro-industry, and are the direct result of aggressive industry lobbying and having powerful senators in their pocket. The rise in calls to poison control for supplements are just one manifestation of this situation.

New Review of Artificial Sweeteners
A new review of research finds a modest but inconsistent benefit from consuming artificial sweeteners over sugar. Their conclusion of a possible backfire effect, however, does not seem to be supported by the studies they review.

