
The DC wants to play PCP on your dime: H.R. 3654 forces Medicare to cover full chiropractic scope of practice
A bill pending before Congress (H.R. 3654) would expand Medicare coverage of chiropractic services to their full scope of practice under state laws. Chiropractors claim they are primary care physicians and want to force Medicare to pay them as such, just like an M.D. or D.O.

Anti-vaccination ideology in chiropractic continuing education and conference (again!)
Yet another chiropractic pediatrics conference features anti-vaccination ideology. Chiropractic institutions approve anti-vaccination CE course content. To protect public health, if chiropractic regulators won't stop this, the states should do it for them.
Medicare proposal covers acupuncture for back pain study participants: A prelude to full coverage?
Medicare coverage of acupuncture is under consideration. A new proposal would provide coverage to Medicare patients participating in studies of acupuncture for back pain. This research would be used in making a final decision.

An Independence Day Tribute to Vaccination
In language that still resonates, Jacobson v. Massachusetts (U.S. Supreme Court, 1905) affirmed state authority to protect health, safety and welfare for the common good with mandatory vaccination despite individual non-medical objections.
“Young blood” infusions: same old snake oil
There's no reliable evidence that an infusion of blood plasma from a young donor will benefit an older person, and there are risks, but Ambrosia Health is selling "young blood" infusions for thousands of dollars anyway. The FDA has taken notice.

Walmart sued for deceiving customers in selling homeopathic remedies
A lawsuit claiming Walmart fraudulently deceives consumers in the sale of worthless homeopathic remedies has been filed by the Center for Inquiry (CFI), acting on behalf of the general public. CFI says co-mingling ineffective homeopathic products with science-based treatments on Walmart's pharmacy shelves and website misleads customers into thinking they are equivalent, when "there is not a shred of credible scientific evidence"...
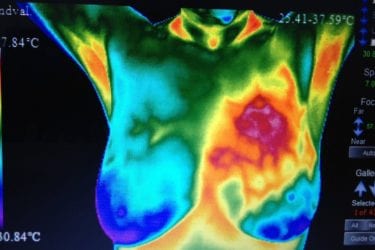
FDA should pull the plug on thermography
The FDA says there's no good evidence that thermography can reliably screen for breast cancer or any other disease. Instead of pursuing the unlawful promotion of thermography for breast cancer detection on a case-by-case basis, the FDA should pull the plug on thermographic devices.

FDA: No CBD in dietary supplements or foods for now, but let’s talk
The FDA reminds everyone that (no matter what your state says) CBD is not a legal ingredient in dietary supplements and foods. The agency is willing to explore changes to the law but unproven claims for CBD health benefits, such cancer cures, will not be tolerated.

Maine considers protecting quacks from accountability to regulators and patients
The Maine Legislature is considering a bill that would put quacks beyond the reach of state healthcare regulatory authorities and leave patients without effective redress for harms.

New FDA rule cracks down on compounded drug ingredients
A new FDA rule will require evidence of safety and effectiveness for substances used in compounded drugs, alarming naturopaths and integrative physicians. Experts have recommended that a number of naturopathic compounding favorites be banned.

