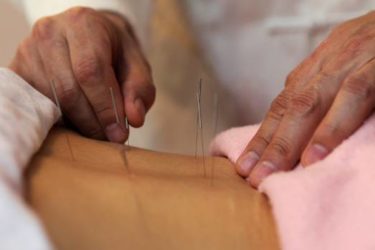
Category: Acupuncture

Yet Another Miscellany of Medical Malarkey
Acupuncture for menstrual cramps, chiropractic for the prevention of domestic terrorism, and more in this miscellany of medical malarkey. Or would you prefer hodgepodge of healthcare hokum?

TCM (Traditional Chinese Medicine): New Developments
Evidence for the efficacy of Traditional Chinese Medicine is scanty, unconvincing, and often fraudulent. China is seeing a resurgence of TCM, even teaching it to children. But in Australia, restrictions are being placed on misleading advertising.

Emergency acupuncture!
For whatever reason, acupuncturists and acupuncture believers think that acupuncture can be useful in emergency situations, be they in the field ("battlefield acupuncture," anyone?) or in the ER. They even do studies purporting to show that. This is yet another of such a clinical trial, albeit larger than usual. Guess what? It doesn't really show what it's advertised to show. I explain...

The closure of major integrative medicine “Crown Jewels”: Terminating the Terminator?
When it comes to expansion and infiltrating medicine, "integrative medicine" has frequently seemed like the Terminator: utterly relentless. Recent setbacks at major integrative medicine "Crown Jewels" resulting in their closure cast that narrative in doubt. However, I never forget that after its seeming destruction, the Terminator always comes back.

Quackery for Kids
A brief rant and a few random observations on quackery for kids.

Corrigendum. The Week in Review for 05/28/2017.
More measles in Minnesota. Yet another form of acupuncture: Snafu. CAM cancer studies are of poor quality. The future of CAM is LSD.

Healthcare reform should ditch mandated coverage of CAM providers
Forced insurance coverage of chiropractic, naturopathic, and acupuncture services is not consistent with the goals of either the ACA or the AHCA. Whatever happens to Obamacare in the U.S. Senate, Section 2706 of the ACA should be repealed.

Quackery infiltrates The BMJ
As quackery in the form of "integrative medicine" has increasingly been "integrated" into medicine, medical journals are starting to notice and succumb to the temptation to decrease their skepticism. The BMJ, unfortunately, is the latest to do so. It won't be the last.
Corrigendum. The Week in Review for 05/21/2017
Choosing CAM leads to bad outcomes the world over. How deep can an acupuncture needle go? Measles continues and Minnesotans and will be welcomed in Texas. Rat rectal stimulation for Science. And more.