Category: Basic Science
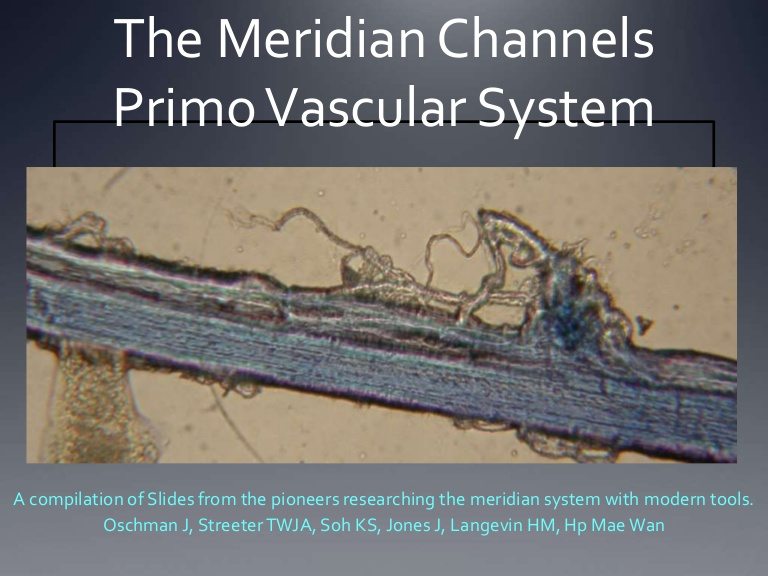
The Primo Vascular System: The N-rays of Acupuncture?
Acupuncture meridians and acupoints are imaginary until proven otherwise. Anatomists have never been able to detect them by microscopy or autopsy, and they are not mentioned in anatomy textbooks. For decades, acupuncturists have been trying to prove that their pre-scientific belief system is grounded in scientific reality. Now they are telling us that acupuncture meridians and acupoints have been discovered in the...

Is there a reproducibility “crisis” in biomedical science? No, but there is a reproducibility problem
Reproducibility is the key to scientific advancement. It has been claimed that we suffer from a "reproducibility crisis," but in reality it is a chronic problem in reproducibility. Here we will look at the scope of the problem and strategies to address it.
“Integrative” medicine versus “alternative” medicine
I’ve written a lot about the language issue with respect to alternative medicine. As I like to put it (at least in shortened form), first there was quackery. Quacks did not like that name at all, and thus was born alternative medicine. And the quacks did think it good—for a while. There was a problem, however. “Alternative” medicine implied (correctly, of course)...
Vaginal Seeding. Ew. That’s nuts. Hmmm, interesting.
Sometimes a headline will cause me to run through a series of reactions in rapid sequence. For example “Mothers facing C-sections look to vaginal ‘seeding’ to boost their babies’ health”: Early studies show that swabbing a mother’s vagina and transferring it to her baby’s mouth, eyes and skin may stimulate microbiome development similarly to babies born naturally – and protect it from...
Sharks Get Cancer, Mole Rats Don’t: Clues to Understanding Cancer
We think of cancer as caused by mutations. Mutations are necessary, but not sufficient, to cause cancer. New research indicates that it’s the body’s response to mutant cells that determines whether cancer will develop. James S. Welsh, MD, a radiation oncologist and researcher, has written a book on the immunology of cancer, Sharks Get Cancer, Mole Rats Don’t: How Animals Could Hold...
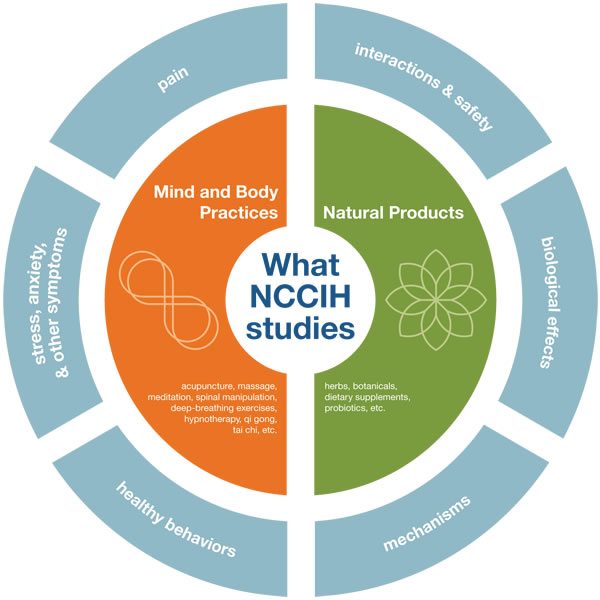
NCCIH Strategic Plan 2016-2021, or: Let’s try to do some real science for a change
It’s no secret that we at Science-Based Medicine (SBM) are not particularly fond of the National Center for Complementary and Integrative Health (NCCIH). Formerly known as the National Center for Complementary and Alternative Medicine (NCCAM) and before that the Office of Alternative Medicine, NCCIH has been the foremost government agency funding research into quackery for the last 24 years, and, of course,...

The hijacking of evidence-based medicine
A hero of the blog, John Ioannidis, worries that evidence-based medicine has been hijacked, and when Ioannidis says something we at SBM listen. But has EBM been "hijacked"?
The Essential Role of Regulation In Human Health and In Ecology: The Serengeti Rules
The doubling time for E.coli bacteria is 20 minutes. With uncontrolled growth, it would take a mere two days for the weight of bacteria to equal the weight of the Earth. What rules determine the actual numbers of bacteria? Why is the world green; why don’t insects eat all the leaves? How does the body maintain homeostasis? What determines the uncontrolled growth...

Zika virus, microcephaly, and calls to bring back DDT (Rachel Carson revisionism edition)
In response to the Zika virus threat, predictably the same group of anti-environmentalists are urging that we bring back DDT and "Spray, baby, spray!" To make their questionable case, they overstate the benefits of DDT, downplay its risks, and engage in some major historical revisionism regarding the legacy of Rachel Carson.
When antivaccine pseudoscience isn’t enough, Bill Maher fawns over Charlie Sheen’s HIV quack
I know I must be getting older because of Friday nights. After a long, hard week (and, during grant season, in anticipation of a long, hard weekend of grant writing), it’s not infrequent that my wife and I order pizza, plant ourselves in front of the TV, and end up asleep before 10 or 11 PM. Usually, a few hours later, between...

