Category: Basic Science
Lyme Testing
I hate those oh hell moments. I was up way too late last night, but who can pass up the opportunity to see Patti Smith playing Horses (and more) for the 40th anniversary of the album. Only 44? Behind the Eagles? No way. I would nudge it up a few more spaces. Hard to believe I was 18 when that album came...
Is scientific peer review a “sacred cow” ready to be slaughtered?
I’ve frequently noted that one of the things most detested by quacks and promoters of pseudoscience is peer review. Creationists hate peer review. HIV/AIDS denialists hate it. Anti-vaccine cranks like those at Age of Autism hate it. Indeed, as a friend of mine, Mark Hoofnagle, pointed out several years ago, pseudoscientists and cranks of all stripes hate it. There’s a reason for...
Of Mice and Men…and Coconut Oil
Editor’s note: This post is a collaborative effort between Grant Ritchey, a Science-Based Medicine semi-regular, and Stephanie Tornberg-Belanger, a co-author of the research paper discussed below and who brought the study to Grant’s attention. We are pleased to welcome Stephanie as a guest contributor to SBM. In his last SBM post, Grant reported on a systematic review of the literature that undermined...
Authority versus science on integrative medicine
David Katz doesn’t much like us here at Science-Based Medicine. In fairness, I can’t say that I much blame him. We have been very critical of his writings and talks over the years, dating back as far as Steve Novella’s deconstruction of one of Dr. Katz’s more infamous statements about using a “more fluid concept of evidence” to Kimball Atwood’s characterization of...
Immunity: More Than Just Antibodies and Vaccines
Since I graduated from medical school, new scientific developments in immunology have been occurring at a prodigious rate. I knew I could use a refresher course, and serendipity dropped one in my mailbox in the form of a review copy of the new book Immunity, by William E. Paul, MD, chief of the Laboratory of Immunology at the National Institute of Allergy...

No, the Nobel Prize does not validate naturopathy or herbalism
This year's Nobel prize is an excellent case study that illustrates the problems with alternative medicine and proving just what science-based medicine can deliver.
“Liquid biopsies” for cancer screening: Life-saving tests, or overdiagnosis and overtreatment taken to a new level?
I’ve written many times about how the relationship between the early detection of cancer and decreased mortality from cancer is not nearly as straightforward as the average person—even the average doctor—thinks, the first time being in the very first year of this blog’s existence. Since then, the complexities and overpromising of various screening modalities designed to detect disease at an early, asymptomatic...
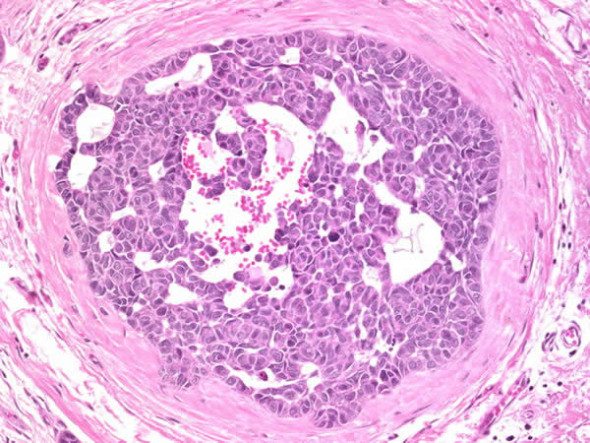
How should we treat DCIS?
I’ve written more times than I can remember about the phenomenon of overdiagnosis and the phenomenon that is linked at the hip with it, overtreatment. Overdiagnosis is a problem that arises when large populations of asymptomatic, apparently healthy people are screened for a disease or a condition, the idea being that catching the disease at an earlier stage in its progression will...