Category: Cancer
Infectious Diseases and Cancer
With apologies to my colleagues, but infectious diseases really is the most interesting specialty in medicine. There are innumerable interesting associations and interactions of infectious diseases in medicine, history, art, science, and, well, life, the universe and everything. ID is so 42. A recent email led me to wander the numerous interactions between infections and cancer. There are the cancers that are...

Personal Care Products Safety Act: Facelift for FDA Regulation or Lipstick on a Pig?
The U.S. cosmetics industry, the largest in the world, is expected to reach $62 billion in revenues in 2016. Yet, despite the fact that its products are regularly applied to, and absorbed by, the body’s largest organ (the skin) and even ingested in small amounts, the cosmetics industry is largely self-regulating. There are over 57,000 different chemicals used in cosmetics. According to...

Diet and exercise versus cancer: A science-based view
Yes, diet and exercise can be useful to prevent some cancers. Unfortunately, they don't prevent all cancers, and the effect size is more modest than often represented. That's not to say that eating right and exercise aren't good. They are, for so many other reasons than cancer. Just don't view them as a panacea for preventing cancer.
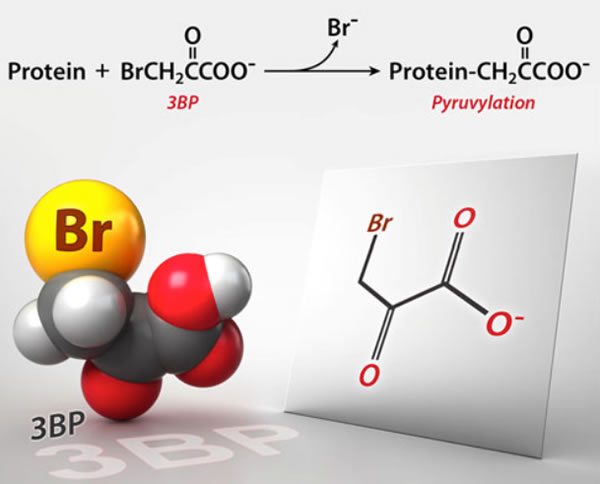
3-Bromopyruvate: The latest cancer cure “they” don’t want you to know about
Why is it that whenever naturopaths and other quacks embrace a new "cancer cure," somehow "they" (whoever "they" are) don't want you to know about it? In this case, it's 3-BP, an actual experimental drug that shows some promise but is by no means ready for prime time (or FDA approval) yet.
The ROCA Screening Test for Ovarian Cancer: Not Ready for Prime Time
Ovarian cancer is relatively rare but deadly. The lifetime risk of ovarian cancer is 1.5% compared to 12% for breast cancer, but it is the 5th most common cause of cancer death for women. Since the ovaries are hidden deep in the pelvis and the symptoms of ovarian cancer are non-specific, the cancer is often advanced by the time it is diagnosed...
Pulsed Electromagnetic Field Snake Oil
Noel Edmonds is a game show host, famous for Britain’s version of Deal or No Deal. As far as I can tell, he has no medical or scientific qualifications at all. This unfortunately has not stopped him from using his celebrity status to offer dubious medical advice via his Twitter feed. Such is the world in which we live. Edmonds tweeted, referring...
False balance about Stanislaw Burzynski and his disproven cancer therapy, courtesy of STAT News
One common theme that has been revisited time and time again on this blog since its very founding is the problem of how science and medicine are reported. For example, back when I first started blogging, years before I joined Science-Based Medicine in 2008, one thing that used to drive me absolutely nuts was the tendency of the press to include in...
No, a rat study with marginal results does not prove that cell phones cause cancer, no matter what Mother Jones and Consumer Reports say
There are certain myths that are frustratingly resistant to evidence, science, and reason. Some of these are basically medical conspiracy theories, where someone (industry and/or big pharma and/or physicians and/or the government) has slam-dunk evidence for harm but conspires to keep it from you, the people. For example, despite decades worth of negative studies, the belief that vaccines are harmful, causing conditions...



The Harm of Integrative Medicine: A Patient’s Perspective
I was diagnosed with cancer and entered treatment, at which point I directly experienced both excellent scientific care, and also the utter nonsense that is alternative medicine, rebranded as integrative medicine. Here are my reflections on the experience.