Category: Cancer
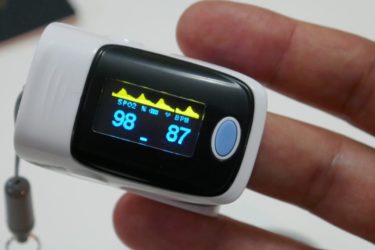
COVID-19 puts the spotlight on an unexpected racial disparity in health care
Evidence increasingly suggests that pulse oximeters, the little finger clips that measure blood oxygen, overestimate the blood oxygenation in Black patients. It's a problem that's been discussed a long time that took a pandemic to bring to public consciousness. How can SBM decrease or eliminate such healthcare disparities?
100% Cure Rate Is Hard to Believe
An experimental cancer drug made 100% of rectal cancers disappear in a small trial, allowing subjects to avoid the standard treatment of chemotherapy and surgery . “Some scientists say these kinds of results have never been seen in the history of cancer research.” 100% is hard to believe; the 95% confidence interval was 74 to 100. Whatever the true percentage, if this...
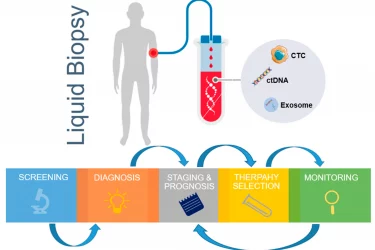
The Role of Liquid Biopsies in Oncology
Liquid biopsies can be used to reduce the amount of chemotherapy used for patients with stage II colon cancer.

Antivaxxers misuse the Defense Medical Epidemiology Database to demonize COVID-19 vaccines
Over the last couple of weeks, a claim that the Defense Medical Epidemiology Database (DMED) shows that COVID-19 vaccines have caused a massive increase in cancer, neurological, and cardiovascular diseases in military personnel has gone viral. A closer look shows that the increases are almost certainly spurious and due to underreporting in previous years.

So-Called Alternative Medicine for Cancer
Edzard Ernst's new book on alternative medicine for cancer addresses cancer prevention, treatment, and palliative care. It is an invaluable, accessible guide to the evidence for each modality.

Avemar: Wheat Germ for Cancer
Avemar is fermented wheat germ. It is claimed to be an effective addition to conventional cancer treatment. The evidence is lacking.
We are not “losing the war on cancer” (belated 2021 edition)
The narrative we hear time and time again is that we are "losing the war on cancer". The latest cancer statistics show that this narrative is not true.
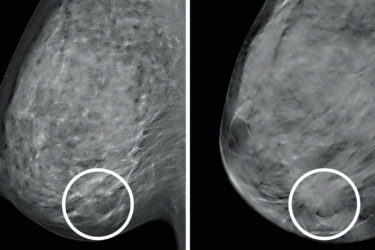
COVID-19 vaccination and screening mammography
Reports of enlarged lymph nodes under the arm after COVID-19 vaccination have led doctors to tweak mammography guidelines. Antivaxxers, unsurprisingly, have tried to weaponize this observation to spread fear and confusion about these vaccines.
Antivaxxers misrepresent a study to falsely claim that COVID-19 vaccines cause cancer
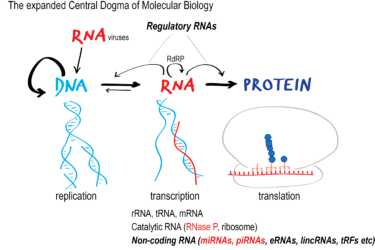
The latest antivaccine propaganda claims that a 2018 research paper published by researchers at Memorial Sloan-Kettering Cancer Center shows that the RNA in the Moderna and Pfizer COVID-19 vaccines can cause cancer. As usual, it's a complete misapplication of a cherry picked study grounded in a lack of understanding of molecular biology. Same as it ever was.
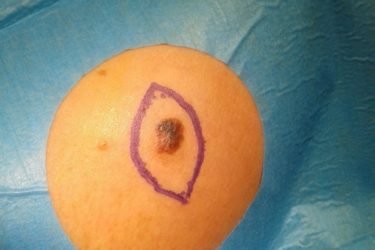
Melanoma: A Pseudoepidemic of Skin Cancer Prompts New Screening Recommendations
There appeared to be an epidemic of melanoma skin cancer, but it seems to be a pseudoepidemic caused by overdiagnosis. Screening everyone with skin exams does more harm than good and can no longer be recommended.

