Category: Chiropractic
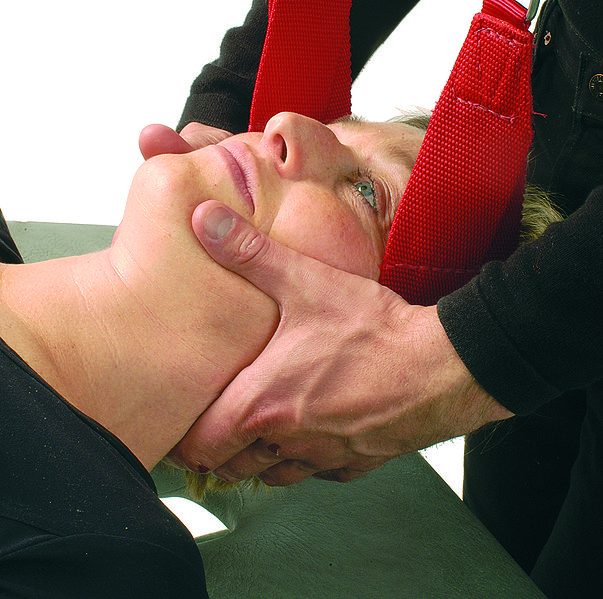
When Headaches Are a Pain in the Neck: Spinal Manipulation vs. Mobilization for Cervicogenic Headache
NOTE: Today we offer a double feature on the treatment of cervicogenic headache. My article is about a study that compared manipulation to mobilization; it is followed by retired chiropractor Sam Homola’s guest article on manipulation for cervicogenic headache. The two posts complement each other and also complement my post from last week on the possible risk of stroke with neck manipulation....
Chiropractic and Stroke: No Evidence for Causation But Still Reason for Concern
Can neck manipulation (by chiropractors or by other practitioners) cause strokes? Many of us think it can, but definitive proof is lacking. A recently published study looked at the available evidence. A systematic review found a small association between stroke and chiropractic care but concluded that the association was spurious and that there was no evidence for causation. My colleagues and I...
Regulating CAM Aussie Style
CAM proponents view National Health Interview Surveys recording the supposed popularity of CAM, an amorphous conflation of anything from conventional medical advice to mythical methods, as an invitation to unleash even more unproven remedies on the public. My interpretation is quite different. I see the same figures as proof that we are doing too little to protect the public from pseudoscience. In...
Oregon Health & Science University SCAM Day
I was looking over a recent class catalog from my alma mater, University of Oregon. I see the Astronomy Department is having a day devoted to astrology, inviting astrologers to talk about their profession. And the Chemistry department is having alchemists give an overview on how to change base metals into gold. And, to green our energy, the Physics Department, where I...
Chiropractic and the Newborn Baby
I had the pleasure of speaking on the topic of chiropractic and the newborn baby earlier this week at a meeting of the Boston Skeptics. There is a video of the talk online for anyone interested in learning more. And if you haven’t yet, please read yesterday’s post on chiropractic and babies by Sam Homola. My introduction to pediatric chiropractic Although I was...
Subluxation Correction: A Chiropractic Treatment for Babies
My article “Pediatric Chiropractic Care: The Subluxation Question and Referral Risk” was published in the 2016 February issue of the journal Bioethics. The abstract summarizes the message of the article: Chiropractors commonly treat children for a variety of ailments by manipulating the spine to correct a “vertebral subluxation” or a “vertebral subluxation complex” alleged to be a cause of disease. Such treatment...

Stem Cells and Chiropractic
My local newspaper is a constant source of topics to blog about. It regularly features ads for untested dietary supplements and for chiropractors who offer non-chiropractic treatments and don’t identify themselves as chiropractors. Recently, a full-page ad for NW Pain Relief Centers trumpeted “Stem Cell Technology Takes Joint Treatment to the Next Level.” It said stem cell treatments could heal and regenerate...
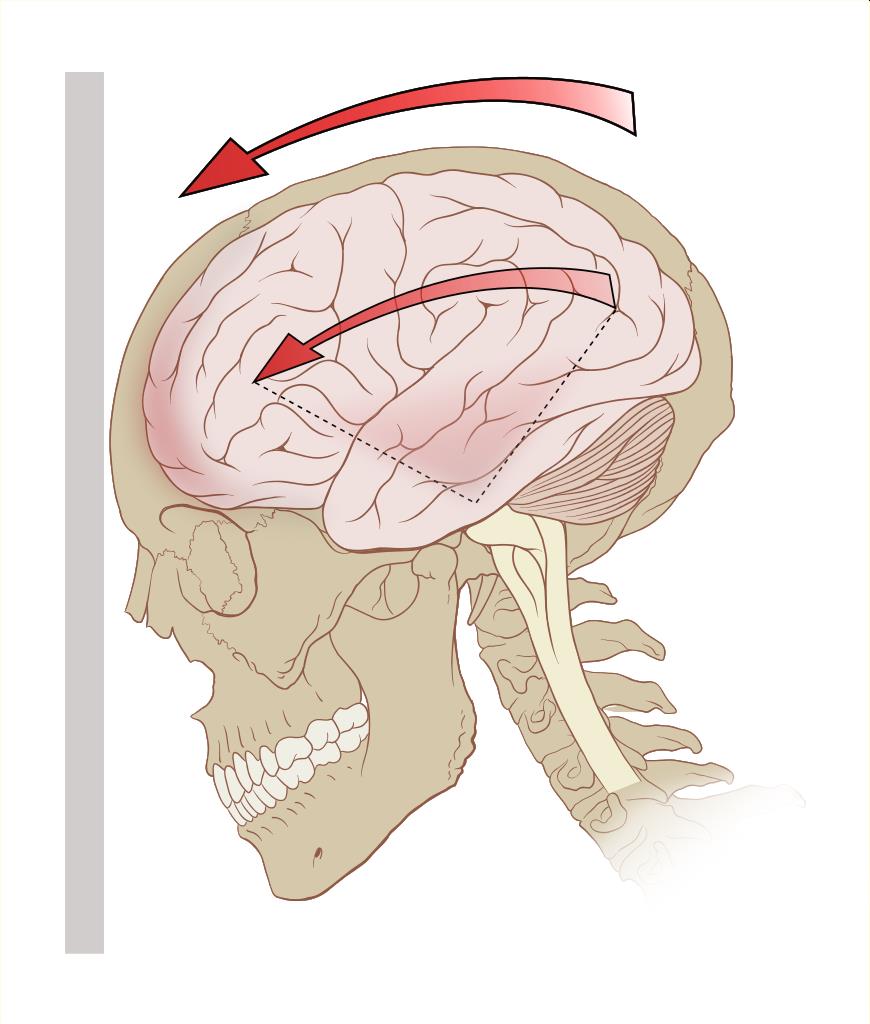
Chiropractors, Naturopaths, Concussions and Senate Bill 1535
Is it a good idea that chiropractors be allowed to clear children to play sports after a concussion? No. It is not a good idea.
Health Savings Accounts: a tax-sheltered way to pay for quackery
If you want money to pay for pseudoscience, but your pesky health insurance company is getting in the way, a Health Savings Account might be just the solution. And if the Health Savings Act of 2016, sponsored by the Big Supplement’s own Senator Orrin Hatch, becomes law, your opportunities will be greatly expanded. First, let’s take a look at Health Savings Accounts...

Did chiropractic neck manipulation kill Katie May?
Well, we’re back. Yes, after having our WordPress database somehow borked to the point where no new posts could be added and no existing posts could be edited since Friday, Science-Based Medicine is back in business—finally! As a result, some of you might have seen this post elsewhere, as it was considered to be somewhat time-sensitive, and I didn’t want to delay,...