Category: Chiropractic

Alternative Reproduction?
Are there effective forms of SCAMs for birth control or reproduction? Of course not.
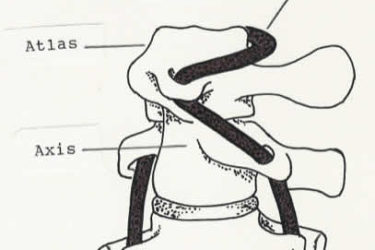
Chiropractic Neck Manipulations in the News
Caitlin Jensen's chiropractor called 911 when she developed alarming symptoms after neck manipulation. She had a heart attack, was pulseless for 10 minutes, and suffered traumatic brain injury. Surgeons found dissections of 4 arteries in the neck. A month later, she remains paralyzed and is still in the ICU.
Anti-vaccination ideology and COVID misinformation in chiropractic continuing education courses: “Plandemic” edition
Chiropractors can still get state-approved continuing ed credit for anti-vaccination courses, with bonus COVID misinformation now added to the curriculum. Plandemic star Judy Mikovits joins the faculty.
The risks associated with alternative medicine
In a new paper, the types and severity of harms from different types of alternative medicine are described.

H.R. 2654 forces Medicare to treat chiropractors and MDs as equals
Chiropractors are deceptively trying to sell H.R. 2654 as expanded Medicare coverage for musculoskeletal conditions. The bill actually mandates that Medicare treat chiropractors and medical doctors as equals, covering anything a chiropractors are authorized to do under their expansive state scope of practice laws.

Science-Based Satire: Area Child Killed by Unwieldy Backpack
Was a child recently murdered by a heavy backpack? Do unwieldy backpacks cause scoliosis and long term general health problems? Should we care what chiropractors have to say about pediatric spinal health? No. This isn't remotely true and honestly I'm a little surprised that you would even ask me that. It's satire.

Chiropractors continue to make claims about chiropractic and COVID-19
Chirorpractors continue to make unsubstantiated claims about COVID-19.

Canadian authorities warn chiropractors and naturopaths against making false COVID-19 claims
Regulators in British Columbia are investigating bogus COVID-19 preventatives and issuing public alerts warning chiropractors and naturopaths against advertising information that is not evidence-based. Other Canadian and U.S. authorities should follow suit to protect the public against pseudoscience.



