Category: Clinical Trials

Should You Take Vitamin D Supplements?
Recent research found that supplemental vitamin D doesn't prevent fractures or have any effect on the diseases it has been claimed to help, and blood tests for vitamin D are useless.

After 15 years of SBM: Lessons learned and what the future holds
Last week, Dr. Novella discussed what SBM has accomplished over the last 15 years. I'm going to discuss lessons learned, what has changed, and remaining huge challenges. Unfortunately, after the pandemic, our position in 2022 reminds me even more than ever of Aragorn at the Black Gate of Mordor, but that does not mean things are hopeless.

What the New York Times gets wrong about puberty blockers for transgender youth
The New York Times recently published an article expressing grave concern about the use of puberty blockers to treat gender dysphoria in transgender adolescents. Unfortunately, the reporting ignored evidence and important context to weave a narrative portraying puberty blockers as far more risky than they actually are.

The Beekeeper: Sentinel Chicken?
Bee venom. Will it help Andy's rheumatism? Doubtful
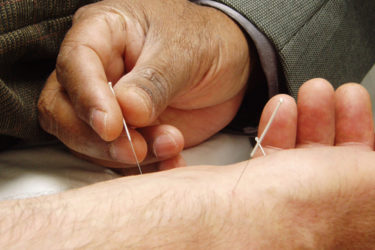
Medicare and Alternative Medicine
Medicare is paying for nonsense.
Aromatase inhibitors and acupuncture in breast cancer: Spinning a negative study, four years later
Four years ago, I wrote about an essentially negative study looking at whether acupuncture could alleviate joint pain caused by aromatase inhibitors, a common treatment for estrogen-sensitive breast cancer. The study's back, and it doesn't look any more positive.
Study – For Lowering Cholesterol, Statins Work, Supplements Don’t
A study comparing a statin drug and six common supplements to placebo shows that only the drug lowers bad cholesterol.

Some Sepsis Stuff
Sepsis interventions. Some don't work and some don't work.
The Pfizer COVID-19 vaccine doesn’t prevent transmission: Antivax disinformation goes viral again
Last week, antivaxxers were all over social media after Tucker Carlson touted a "revelation" that the phase 3 clinical trial used to support licensure of the Pfizer COVID-19 vaccine didn't examine its ability to block transmission as meaning that its inability to block transmission had been "covered up". It wasn't, and antivaxxers are ignoring everything we've learned over the last two years...


