Category: Clinical Trials

Ivermectin is the new hydroxychloroquine, take 3: Conspiracy theories vs. science
Last month, I discussed why ivermectin is the new hydroxychloroquine:, basically a “miracle cure” that isn’t. Since then, conspiracy theories about its being "suppressed" have continued to bump heads with the science showing that, at the very best, evidence for its efficacy is very weak and, at the worst, the drug is useless.

Abigail Shrier’s Irreversible Damage: A Wealth of Irreversible Misinformation
A critical, science-based analysis of Abigail Shrier's book Irreversible Damage.

Ivermectin is the new hydroxychloroquine, take 2
A few months ago, Scott Gavura wrote about how the veterinary deworming drug ivermectin has become the new hydroxychloroquine in that it is being promoted as a highly effective treatment against COVID-19—and by many of the same people who previously promoted HCQ—despite evidence that is, at best very weak and at worst completely negative. Unfortunately, with the publication of two new and...

No evidence, no problem: A closer look at the aducanumab approval
Why did the FDA approve aducanumab, a drug that hasn't been shown to work?
A Blood Test for Fibromyalgia?
The FM/a test is advertised as a definitive test to diagnose fibromyalgia. It isn't definitive. It is expensive. It has not been shown to change patient outcomes.
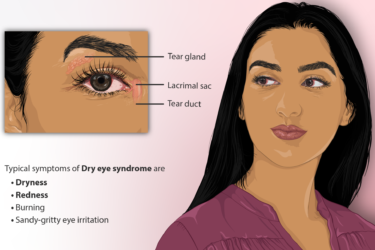
Eye Drops for Dry Eyes
I could have chosen a prescription eye drop for my dry eyes. I decided not to. Here's why.
To unblind or not to unblind? That is the question about clinical trials of COVID-19 vaccines
Antivaccine alternative health tycoon Joe Mercola claims that the unblinding of participants in the clinical trials of Moderna and Pfizer COVID-19 vaccines was intended to "blow up the trials" and undermine the science, making it impossible ever to identify long term adverse events. What he's really doing is deceptively oversimplifying complex ethical and scientific issues surrounding these trials in the middle of...
Catgut Acupuncture
Catgut acupuncture is but one example of how acupuncture's basis in pseudoscience provides an infinitely malleable template for fabricated mechanisms of action and feigned health benefits.
Ivermectin is the new hydroxychloroquine
Ivermectin has been touted as a potential antiviral to treat COVID-19 infections. There is no good evidence it is effective.

A New Medication to Combat Obesity
New study in The New England Journal of Medicine finds impressive evidence that weekly semaglutide injections produce clinically significant weight loss as well as many other benefits, approaching the improvements seen with weight loss surgery. Not a definitive answer to obesity, but a very encouraging step in the right direction. Science works.

