Category: Diagnostic tests & procedures
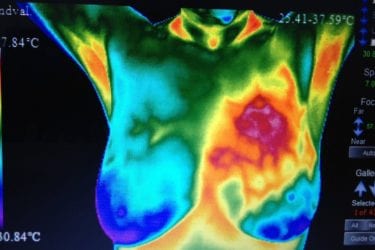
FDA should pull the plug on thermography
The FDA says there's no good evidence that thermography can reliably screen for breast cancer or any other disease. Instead of pursuing the unlawful promotion of thermography for breast cancer detection on a case-by-case basis, the FDA should pull the plug on thermographic devices.
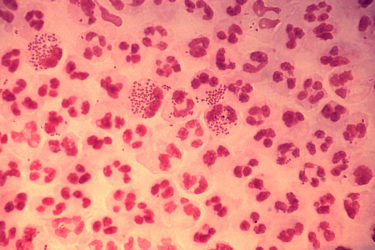
SmartJane Test of Vaginal Health: Clever Marketing, Questionable Science
uBiome claims that its SmartJane test's proprietary technology empowers customers to assess their own vaginal health. The company is being investigated for fraudulent billing practices, and the rationale for the test makes no sense.
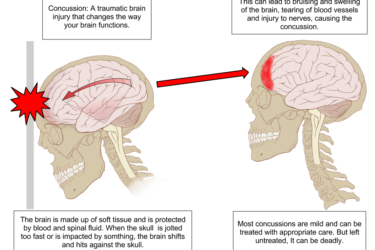
Chiropractor Treating Concussions for Earlier Return to Play
A chiropractor is using questionable diagnostic and therapeutic measures to return athletes to play sooner after a concussion. Not a good idea.
Experts slam CAM lab tests, call for better regulation
Experts review the evidence and find that common CAM lab tests have "little or no clinical benefit" and are "a potential risk to patient safety." Regulatory reform is urgently needed to protect the public.
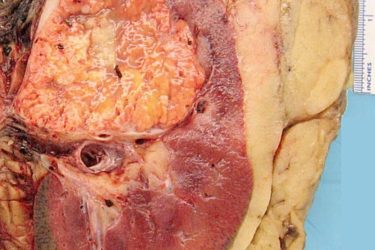
Kidney Cancer and Incidentalomas
Kidney cancer diagnoses are increasing but there has been no increase in mortality or rate of metastases. Kidney cancer is most often diagnosed as an incidental finding on a CT scan that was done for unrelated reasons. Treatment may not always be needed.
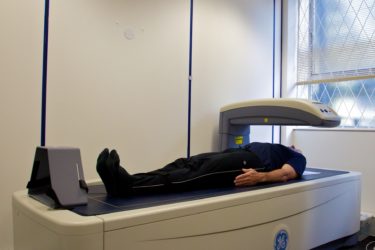
Osteopenia: When Does Decreased Bone Density Become a Disease Requiring Treatment?
Osteoporosis is routinely treated with bisphosphonates to prevent fractures. A new study suggests that osteopenia should be treated too. But questions remain.

Functional medicine: Reams of useless tests in one hand, a huge invoice in the other
"Functional medicine" preaches the "biochemical individuality" of each patient, which is why one of its key features is that its practitioners order reams of useless lab tests and then try to correct every abnormal level without considering (or even knowing) what these abnormalities mean, if anything. So they make up fake diagnoses and profit.
Can DNA testing predict your response to drugs?
Can your genes really predict how you will metabolize certain medications? The FDA has approved the first direct-to-consumer test that claims to do this. How meaningful are the findings?



Vertigo Voodoo: A Crazy-Sounding Cure That Actually Works
A sequence of positional changes sounds like voodoo, but is actually an effective way to cure benign paroxysmal positional vertigo (BPPV).