Category: Herbs & Supplements

I Was Wrong about Protandim
A seriously flawed Protandim study seemed to show that side effects were no more common than with placebo. Actually, they were almost twice as common. The researchers were looking at the wrong numbers and didn't even add correctly.

Turpentine, the Fountain of Youth According to Dr. Jennifer Daniels
Jennifer Daniels says turpentine is the Fountain of Youth, able to cure many ailments, both real and imaginary. It isn't; it's a poison with no recognized benefits for human health.
Update on ASEA, Protandim, and dōTERRA
Multilevel marketing distributors of dietary supplements and essential oils point to studies that they think constitute evidence that their products work. They don't understand why those studies are inadequate.
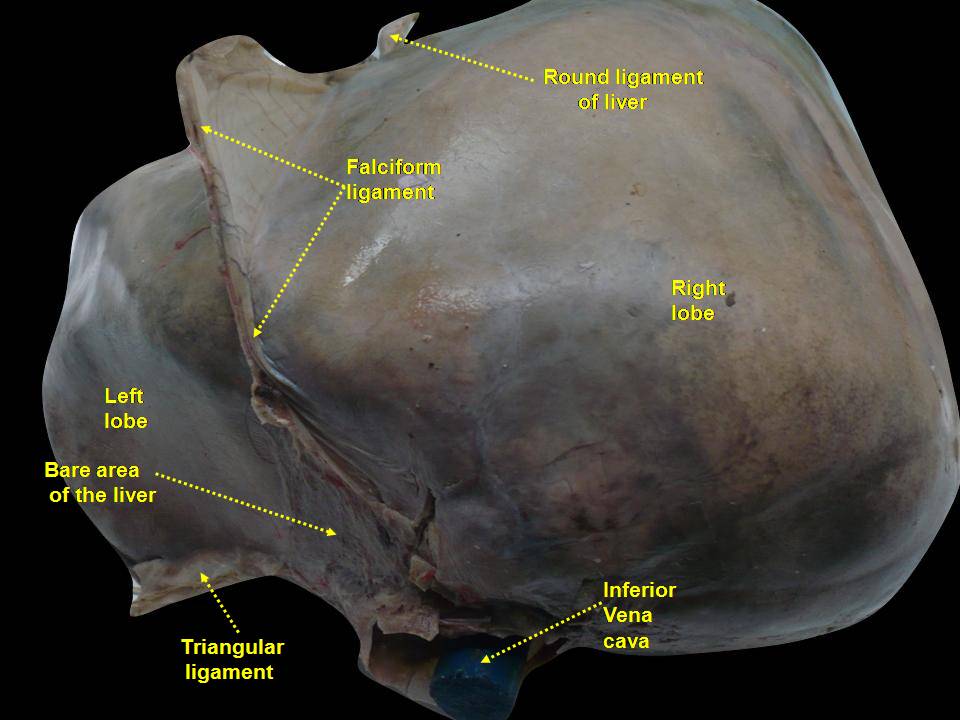
Liver cancer, naturally
Aristolochic acid, a highly toxic substance naturally found in some traditional herbal medicines, may be a significant cause of liver cancer.

ASEA – Still Selling Snake Oil
ASEAs marketing practices, in my opinion, are clearly deceptive. They use a lot of pseudoscientific claims representing the epitome of supplement industry misdirection and obfuscation. They use science as a marketing tool, not as a method for legitimately advancing our knowledge or answering questions about the efficacy of specific interventions.

AAFP: Functional Medicine lacks supporting evidence; includes “harmful” and “dangerous” treatments
The American Academy of Family Physicians (AAFP) found Functional Medicine lacking in evidence and said some treatments are harmful and dangerous. The AAFP is right and should stick to its conclusions.
Australia ends insurance subsidies for naturopathy, homeopathy, and more
The Australian government has eliminated the insurance subsidy for 17 alternative health practices due to a lack of evidence for efficacy. This is a win for medicine and Australian taxpayers.

Preying on the Vulnerable: Electrodiagnostics, Bach Flower Remedies, and Sound Therapy for Autism, ADHD, and Learning Problems
Karyne Jeanne Richardson offers a ridiculous program of electrodiagnosis, flower remedies, and fractal sound to treat autism and other disorders. There are science-based autism programs that work; it is unfortunate when parents subject their autistic children to onerous, expensive, time-consuming, useless treatments based on pseudoscientific claims and false promises.
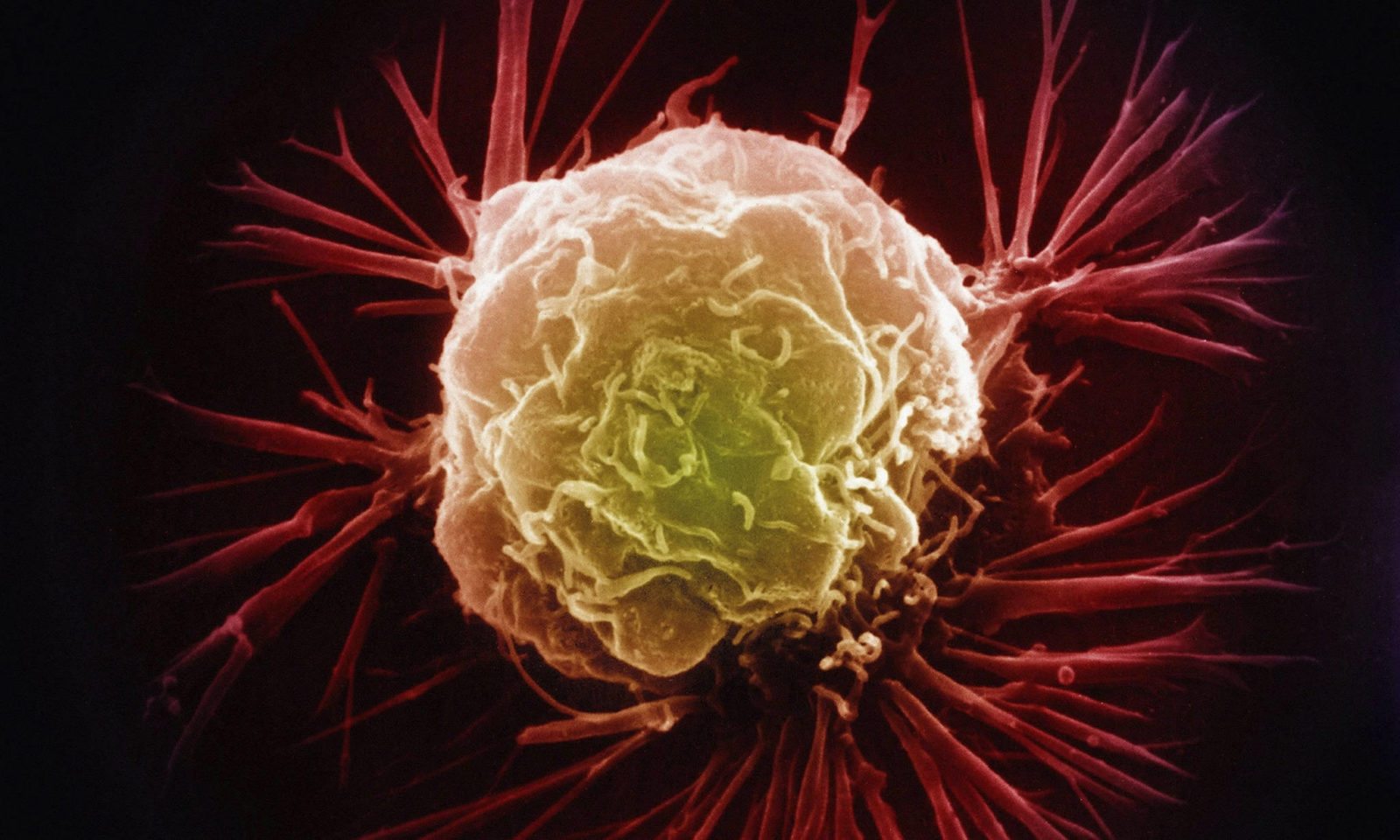
Complementary and Alternative Medicines and Cancer
Does complementary and alternative medicine offer any meaningful benefits to cancer patients?

Faith and Supplements – B17
Amygdalin is a toxic snake oil dating back to 1830, but it is still sold today with a combination of supplement industry deception, faith, and conspiracy theories.

