Category: Neuroscience/Mental Health
Neurological Manifestations of COVID
The more we study COVID, the more apparent it is that neurological symptoms are common and can be long lasting.

Genetic Testing for Selection of Psychotropic Medications
GeneSight is a blood test to determine which neuropsychiatric medications are indicated for an individual based on genetic analysis. The test is expensive and not likely to be helpful for most patients.

Mayim Bialik’s Neuriva Commercials Make Questionable Claims
Mayim Bialik is a neuroscientist. In her TV commercials for Neuriva Plus she asserts that it is backed by strong science. I don't think so.

Irreversible Damage to the Trans Community: A Critical Review of Abigail Shrier’s Irreversible Damage (Part One)
Irreversible Damage, a controversial 2020 book by Abigail Shrier, has enjoyed renewed attention in the last several weeks. Shrier appeals to her audience’s emotions by voicing their deepest fears to create uproar against an already marginalized community. The claims presented do not meet scientific rigor, yet have been praised and upheld by many, effectively pushing back against equal rights for gender minorities,...
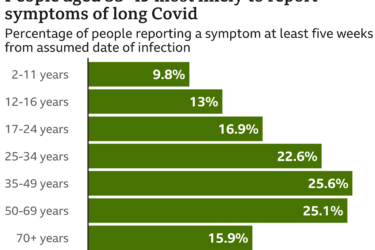
Long COVID
Medical experts are just starting to bring long COVID into focus, but there is still much we don't know.
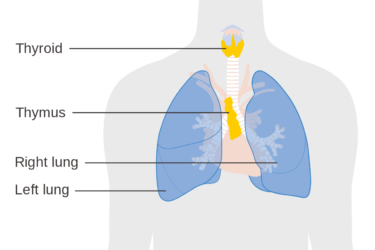
Who Is Amy B. Scher?
Amy B. Scher is a proponent of energy medicine and things like astrology and homeopathy. She claims to be a "science geek," but how could anyone who understands science think that tapping on the breastbone will fix the thymus?

Visual Stress
The Opticalm Clinic claims to diagnose and treat visual stress with colored lenses and other aids. Visual stress is a poorly defined, questionable condition and Opticalm's claims are not backed by scientific evidence.

Shooting the Messenger: Activists Persecute Scientists Whose Findings They Don’t Like
Alice Dreger's book recounts many instances of shooting the messenger, when scientists were persecuted for research findings that activists found objectionable. Social justice matters, but it should rely on science and reality, not ideology.

Psychic Mediums and Grieving Children
Self-proclaimed psychic mediums find a new way to exploit vulnerable children.