Category: Pharmaceuticals
Hormone Replacement Therapy for Menopausal Symptoms: Setting the Record Straight
Whether you call them hot flashes or “power surges,” the symptoms of menopause can be very distressing. They were routinely treated with hormone replacement therapy (HRT) until the Women’s Health Initiative study in 2002 persuaded many patients and doctors to abandon that treatment. The results of that study were misunderstood by some and questioned by others, and there continues to be confusion...
More drugs, more supplements, and potentially more problems
Early in my career I was fortunate to be offered a role as a hospital pharmacist, working on an inpatient ward along with physicians, nurses, and a number of other health professionals. My responsibilities included conducting a detailed medication review with each newly admitted patient. We would sit together, often with family members, going through what was sometimes a literal garbage bag...
Testing Testosterone Treatments
Ponce de Leon is said to have been looking for the Fountain of Youth when he explored Florida. That’s only a myth. Now there’s a new myth, that testosterone supplements are a Fountain of Youth for aging men. Men are urged to get their testosterone levels checked if they have any of a long laundry list of vague symptoms. Anti-aging clinics promote...

The hijacking of evidence-based medicine
A hero of the blog, John Ioannidis, worries that evidence-based medicine has been hijacked, and when Ioannidis says something we at SBM listen. But has EBM been "hijacked"?
Why Antibiotic Use Scares Me
Editor’s note: Today we present a guest post from fourth-year medical student Joshua Horton, about the looming problem of antibiotic resistance. Welcome! I read a study recently that alarmed me: acute bronchitis is a condition that rarely requires antibiotics, but three quarters of patients presenting with this condition receive a prescription for antibiotics. Even more worrisome, this statistic has not changed in...

Statin Side Effects
How bad are the side effects of statin use? A recent article on the subject suggests that they are not bad, comparable to the base rate in the population.
Patient Beware: Off-label drug promotion by pharmaceutical companies
Pharmaceutical companies and their sales reps can distribute information, such as medical journal articles, about unapproved (“off-label“) uses of their drugs as long as they adhere to FDA guidelines. However, the FDA takes the position that this information must be distributed separately from information that is “promotional in nature,” i.e., for marketing purposes, a position that is now open to question. Off-label...

Stem Cells and Chiropractic
My local newspaper is a constant source of topics to blog about. It regularly features ads for untested dietary supplements and for chiropractors who offer non-chiropractic treatments and don’t identify themselves as chiropractors. Recently, a full-page ad for NW Pain Relief Centers trumpeted “Stem Cell Technology Takes Joint Treatment to the Next Level.” It said stem cell treatments could heal and regenerate...
Pseudoscience sneaks into Ohio guidelines for non-drug pain treatment
Ohio recently issued Acute Pain Prescribing Guidelines as part of an effort to reduce the epidemic of opioid abuse and death from overdose. They were drafted under the auspices of the Governor’s Cabinet Opiate Action Team (GCOAT), assisted by medical organizations and other groups. The guidelines include recommendations for non-pharmacologic treatment, a typical feature of pain treatment guidelines and a worthy effort...
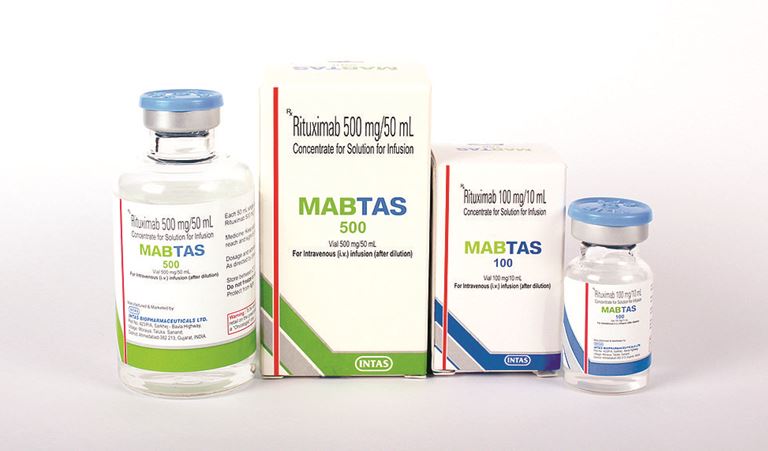
Chronic Fatigue Syndrome: Rituximab Revisited
Three years ago I wrote about an experimental treatment for chronic fatigue syndrome (CFS): rituximab (brand name Rituxan). I was concerned that doctors who offered it, like Andreas Kogelnik, were jumping the gun by offering it before the evidence was in, and that they might be putting patients at risk. A correspondent who has been following the CFS forums asked me to...

