Category: Science and Medicine
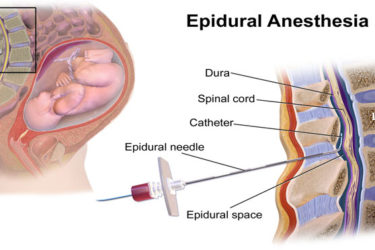
Epidural Labor Analgesia Not Linked to Autism Says New and Improved Study
A new and improved study investigating a potential link between epidural analgesia during labor and autism found no connection. That's great news for mothers and babies.

Some essential oils may trigger seizures
Some essential oils appear to trigger seizures in people with no history of epilepsy.

Another In a Pattern of Really Stupid Marketing Videos, This One Claiming Tinnitus Has Nothing to Do with the Ear and Is 100% Curable.
This really stupid video was an insult to my intelligence. Nothing in it can be believed. They claim tinnitus has nothing to do with the ears and they sell a 100% effective dietary supplement mixture supposedly developed by MENSA with government funding. It has never been clinically tested. No, there is no cure for tinnitus.

Deaths and Excess Deaths in Brazil
By misinterpreting excess mortality statistics, Nobel Laureate Michael Levitt minimizes the significance of the COVID-19 pandemic in Brazil (and also America).

Christian Elliot’s “18 Reasons I Won’t Be Getting a Covid Vaccine”: Viral antivaccine misinformation
Christian Elliot is a self-proclaimed "natural health nerd" and entrepreneur who recently published 18 reasons why he wouldn't take the COVID-19 vaccine. Unfortunately, it's viral disinformation based on conspiracy theories, bad science, pseudoscience, and nonsense.
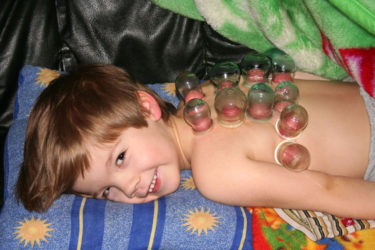
Adverse Events Linked to Pediatric “Alternative Medicine” in the Netherlands
A study out of the Netherlands documented pediatric adverse events associated with complementary and alternative medicine over three years. Thankfully there weren't a lot of kids harmed, but when there is no potential benefit from an intervention, even one is way too many.

COVID-19 vaccines versus “purity of essence”
Antivaxxers frequently make the false claim that mRNA-based COVID-19 vaccines "permanently alter your DNA". These claims are really a concern about "impurifying" their "purity of essence".

Antivaxxers, COVID-19 vaccines, and “hacking the software of life”
Antivaxxers and COVID-19 conspiracy theorists were always going to spin conspiracies about COVID-19 vaccines. Unfortunately, some scientists have made it so much easier for them by having likened mRNA vaccines to "hacking the software of life" and being unclear on what gene therapy is.

The Residency Match is Broken
The National Resident Matching Program (Match), the program to align med school applicants with their preferred residency program, is broken and filled with disincentives. The fix might be easy.
More Data Supports Delayed Antibiotic Prescribing for Kids with respiratory infections
Overuse of antibiotics is a big problem. New data supports delaying that prescription for kids with respiratory infections.

