Category: Science and Medicine
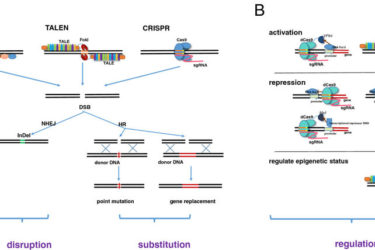
CRISPR vs. TALEN
There are more than one genetic engineering technologies available. Here's a comparison.

All science denial is a form of conspiracy theory
Regular readers of this blog know that many forms of quackery and science denial have conspiracy theories associated with them, but a further examination suggests that all forms of science denial are a form of conspiracy theory. In the middle of a deadly pandemic, science denial represents a form of conspiracy theory with potentially deadly consequences.
Science-Based Satire: Implantable Desubluxators Revolutionize Chiropractic Care
Have chiropractic scientists developed an implantable device that will detect and treat subluxations? Are there companies that monitor these devices in order to alert patients and to arrange for 24-7 emergency adjustments? No. There absolutely are not. This is satire.
Germ theory denial in the age of the COVID-19 pandemic
As hard as it is to believe, in the middle of a global pandemic that's claimed so many lives and so thoroughly disrupted society, there are people who still deny germ theory. How can this be?

The Guardian and the “Cult” of Online Chiropractic
Over the past few years, a handful of chiropractors have gone viral because of aggressive neck adjustments that make a loud crack and provide a quick thrill for viewers of their YouTube videos. A recent article in The Guardian discussed the phenomenon, but it doesn't go far enough.

Homeopathy Declining in Germany
Homeopathy is on the decline in Germany and elsewhere, partly due to the dedicated action of skeptics.
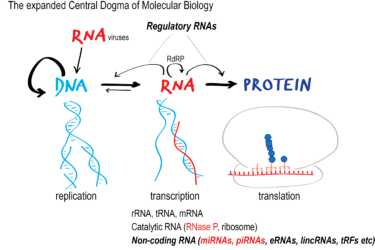
No, the Moderna and Pfizer RNA vaccines for COVID-19 will not “permanently alter your DNA”
With the new mRNA vaccines developed by Pfizer/BioNTech and Moderna likely to be available soon, antivaxxers have been ramping up the fear mongering. Their latest claim is that mRNA vaccines will "permanently alter your DNA" or even "make you transhuman." Such claims rest on an utter ignorance of the totality of what we know about the biology of DNA, RNA, and how...



2020 – The Good and the Bad
What 2020 has taught us about the power of science and the harm of pseudoscience.