Category: Science and Medicine
In the age of the COVID-19 pandemic, can we trust the CDC and FDA any more?
Since the COVID-19 pandemic reached the US, increasing concern has been expressed about the politicization of the CDC and FDA due to pressure from the Trump administration to downplay the severity of the pandemic and push out treatments and a vaccine as fast as possible, potentially at the expense of safety. This has led me to a disturbing question: Can I trust...

Did the “Benadryl Challenge” Kill an Oklahoma Teen?
Did a dangerous new TikTok "challenge" result in the death of a 15-year-old teenager from Oklahoma? Probably not, but Benadryl is still a bad drug and parents should discuss the dangers of social media with their young children.

COVID in Children
Recent evidence suggests children can be carriers of SARS-CoV-2, which has implications as schools reopen this Fall.
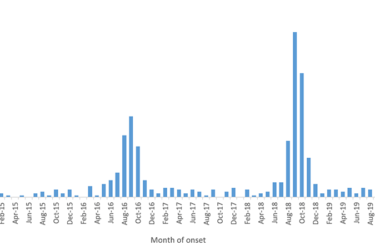
CDC Issues Warning: Be on the Lookout for a Surge in Pediatric Paralysis Cases This Fall
The CDC is warning parents and pediatric medical professionals to be on the lookout for a potentially devastating viral disease this fall. It isn't the novel coronavirus, but the impact of the pandemic might make things worse...or better.

Science-Based Satire: Area Child Killed by Unwieldy Backpack
Was a child recently murdered by a heavy backpack? Do unwieldy backpacks cause scoliosis and long term general health problems? Should we care what chiropractors have to say about pediatric spinal health? No. This isn't remotely true and honestly I'm a little surprised that you would even ask me that. It's satire.

Emerging Evidence of Intrauterine SARS-CoV-2 Infections
New evidence supports the potential for intrauterine spread of SARS-CoV-2 to a developing fetus. It's uncommon, but something to take seriously. Also some good news from the AAP regarding the care of babies born to mothers with COVID-19!

The English (Bulldog) Patient: What A Travesty of Canine Health Teaches us About Cognitive Dissonance
Bulldogs are cute, loveable, and borderline an abuse to breed. Their adorable faces are the result of intense selective pressure that is accompanied by a large number of misery-inducing health conditions for the pet, and cognitive dissonance for the owner.
COVID-19 “super-spreaders” and “super-spreading events”: The controversy
Evidence is emerging suggesting that COVID-19 does not spread equally. A minority of infected individuals seem to spread the virus easily to many people, while most infected individuals spread it to few others or no one at all, likely through a combination of circumstance, environment, and possibly biology. Why is this, and what does it mean for coronavirus containment strategies?

A Poorly Conceived Study Fails to Prove Ayurveda Works
Quackery is alive, well, and government-supported in India, as demonstrated by a terrible study of Ayurveda.

The Questionable Ethics of Medical Grade Nonsense: Chinese Herbal Medicine and Kawasaki Disease
A toddler in China with Kawasaki disease was treated with herbs and potions rather than science, and is extremely lucky to have survived without serious complications.

