Category: Science and Medicine
April Fool Cannot Surpass SCAM
It’s April Fools’ day in the US of A. One of the internet traditions is to come up with a story that is weird or unlikely, but not so weird or unlikely that it is not believable, in order to fool people that the story is real. I gave it the old SBM try, I really did, but I couldn’t do it....
Audio Therapy for Postoperative Pediatric Pain: Randomized Controlled Nonsense
In January of 2015, a study on “the effect of audio therapy to treat postoperative pain in children” performed at Lurie Children’s Hospital and published in Pediatric Surgery International made the media rounds. It was the typical story where numerous news outlets further exaggerated already exaggerated claims made in a university press release, in this case Northwestern University in Chicago. Some of...
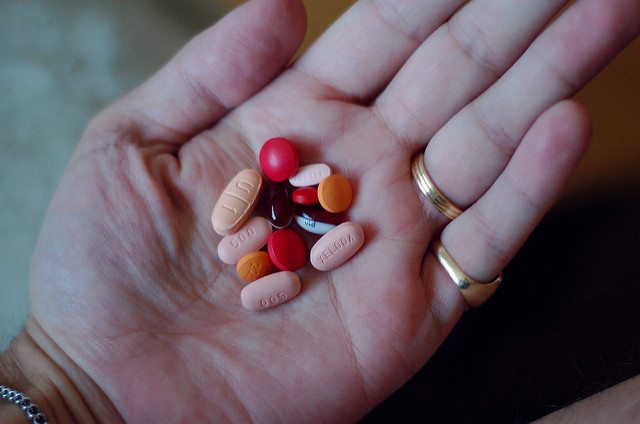
More drugs, more supplements, and potentially more problems
Early in my career I was fortunate to be offered a role as a hospital pharmacist, working on an inpatient ward along with physicians, nurses, and a number of other health professionals. My responsibilities included conducting a detailed medication review with each newly admitted patient. We would sit together, often with family members, going through what was sometimes a literal garbage bag...
Why Antibiotic Use Scares Me
Editor’s note: Today we present a guest post from fourth-year medical student Joshua Horton, about the looming problem of antibiotic resistance. Welcome! I read a study recently that alarmed me: acute bronchitis is a condition that rarely requires antibiotics, but three quarters of patients presenting with this condition receive a prescription for antibiotics. Even more worrisome, this statistic has not changed in...
Oregon Health & Science University SCAM Day
I was looking over a recent class catalog from my alma mater, University of Oregon. I see the Astronomy Department is having a day devoted to astrology, inviting astrologers to talk about their profession. And the Chemistry department is having alchemists give an overview on how to change base metals into gold. And, to green our energy, the Physics Department, where I...
Ezekiel Stephan: Another Pediatric Death by World View
Reports of a disturbing chain of events that ended in the likely preventable death of a 19-month-old Canadian child have made the rounds this week. The case was discussed by friend of Science-Based Medicine Orac (who I believe is some kind of a protocol droid) on Respectful Insolence two days ago. But even if you’ve read that excellent post, please continue reading...
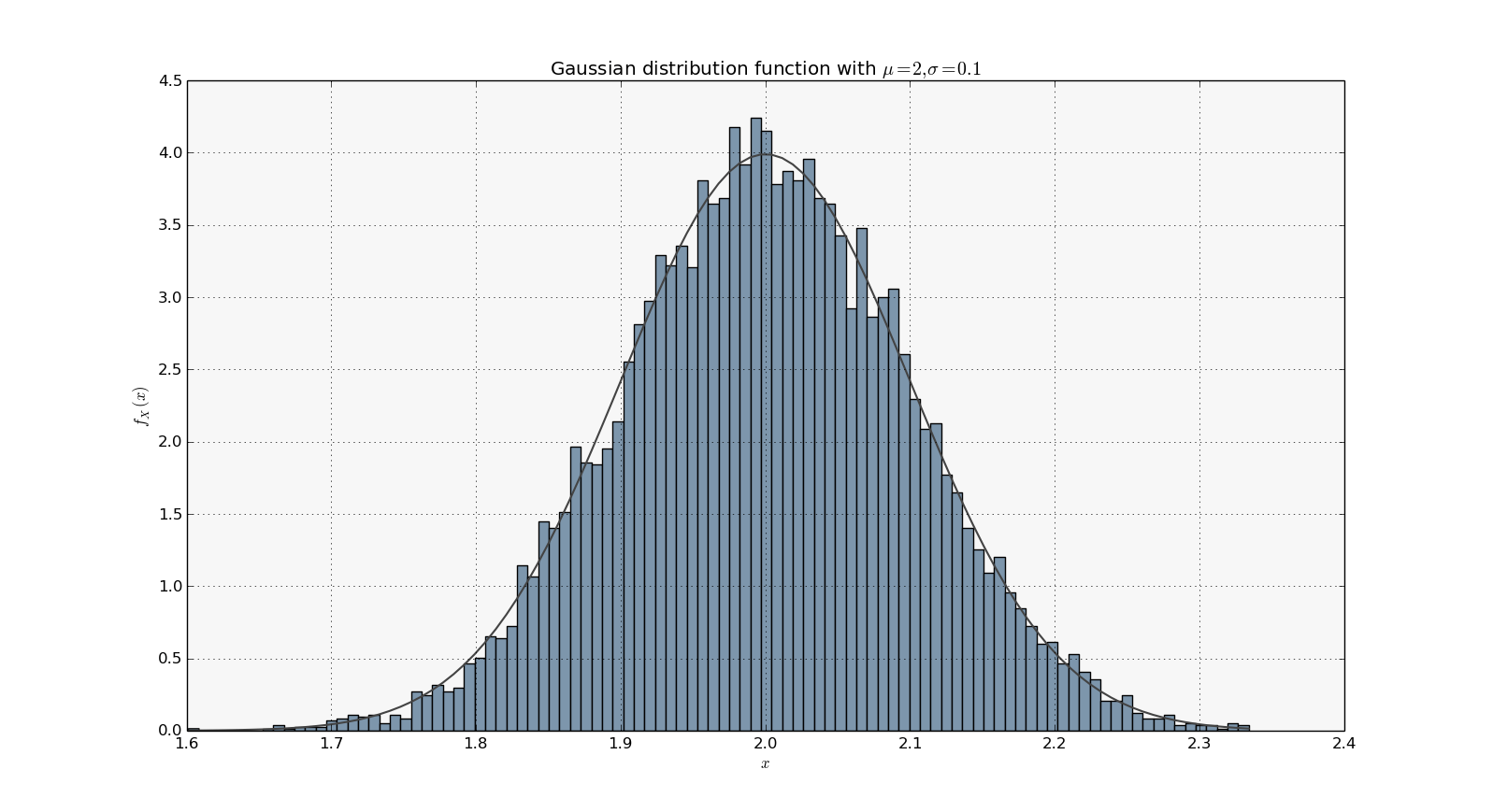
P Value Under Fire
The greatest strength of science is that it is self-critical. Scientists are not only critical of specific claims and the evidence for those claims, but they are critical of the process of science itself. That criticism is constructive – it is designed to make the process better, more efficient, and more reliable. One aspect of the process of science that has received...
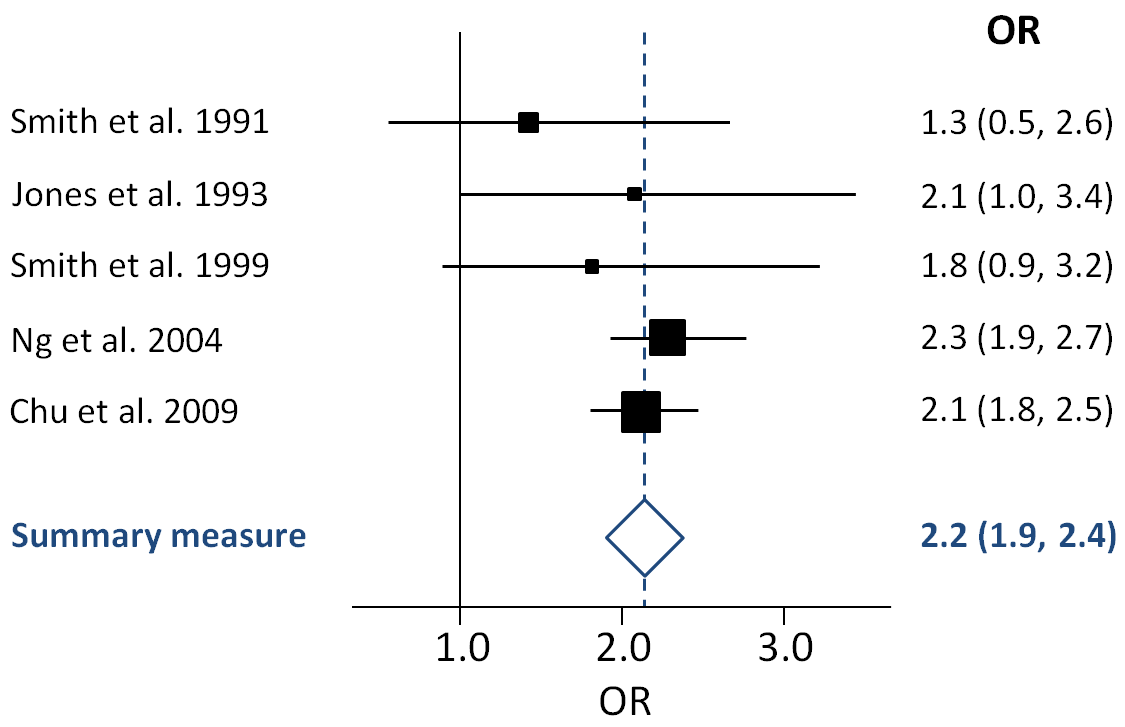
Reporting results from clinical trials is vital for science-based medicine
Clinical trials must report on their outcomes, irrespective their results. Doctors and their patients need all the information, not just the good news stories, to make informed decisions.
Chiropractic and the Newborn Baby
I had the pleasure of speaking on the topic of chiropractic and the newborn baby earlier this week at a meeting of the Boston Skeptics. There is a video of the talk online for anyone interested in learning more. And if you haven’t yet, please read yesterday’s post on chiropractic and babies by Sam Homola. My introduction to pediatric chiropractic Although I was...
Subluxation Correction: A Chiropractic Treatment for Babies
My article “Pediatric Chiropractic Care: The Subluxation Question and Referral Risk” was published in the 2016 February issue of the journal Bioethics. The abstract summarizes the message of the article: Chiropractors commonly treat children for a variety of ailments by manipulating the spine to correct a “vertebral subluxation” or a “vertebral subluxation complex” alleged to be a cause of disease. Such treatment...

