Category: Science and Medicine
Traditional Chinese Pseudo-Medicine Hodgepodge
As I have noted before, more is published on acupuncture and traditional Chinese pseudo-medicine than the other SCAM. Here are some of the articles that drew my attention. Captain Hook and acupuncture Here is one of the more curious articles on acupuncture I have yet to find, “Psychophysical and neurophysiological responses to acupuncture stimulation to incorporated rubber hand.” I did not know...
Reporting Research Misconduct
Perhaps one of the greatest threats to the enterprise of Science-Based Medicine is research fraud and misconduct. Rigorous research methods can be used to minimize the effects of bias, but when those methods themselves are the problem there is no easy fix. Related to this is the need for transparency. When fraud or misconduct is uncovered it erodes confidence in the system...
Hot-Zone Schools and Children at Risk: Shedding light on outbreak-prone schools
The subject of parental vaccine refusal and the impact that has on disease outbreaks has been covered many times on SBM and elsewhere. I apologize to our readers who are growing tired of the subject, but there is perhaps no subject more deserving of focus and repetition. There’s also an important angle to the discussion that I’ve written on previously and which...
Are skin-lightening glutathione injections safe and effective?
Naturopaths advertise injections claimed to lighten skin. Are these products safe and effective?
Does a Common Treatment for Childhood Constipation Cause Autism?
Last week an article published by the New York Times entitled “Scrutiny for Laxatives as a Childhood Remedy” made the rounds. The article raised the question of a possible link between the use of a popular over-the-counter laxative, PEG (polyethylene glycol) 3350, and neurological or psychiatric problems in children. This wasn’t the first time this particular journalist wrote a piece on this...
Skeptic’s Guide to Debunking Claims about Telomeres in the Scientific and Pseudoscientific Literature
The New Year starts with telomeres as the trendiest of trendy biomarkers. As seen in Time, telomeres are the means to monitor our well-being so we can protect ourselves from all sorts from threats, including early death. A skeptic needs to do considerable homework in order to muster the evidence needed to counter the latest exaggerated, premature, and outright pseudoscientific claims about...
Neuroscience and Destiny
A newly-published review of neuroscience research looking at the predictive value of functional and anatomical imaging raises interesting questions about the role of such studies in learning, psychiatric treatment, and even the treatment of criminals. “Prediction as a Humanitarian and Pragmatic Contribution from Human Cognitive Neuroscience” by Gabrieli, Ghosh, and Whitfield-Gabrieli and published in Neuron, does a thorough job of explaining the...
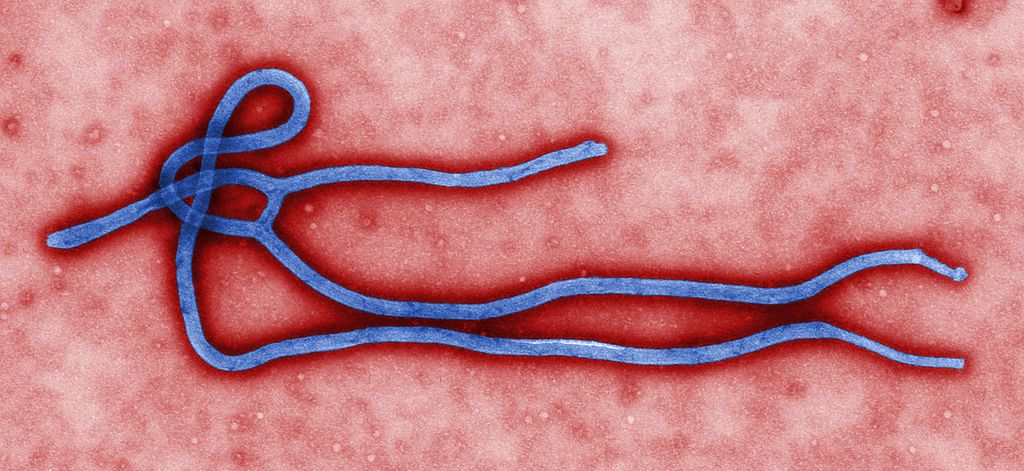
Is the Ebola Crisis a Reason to Skip RCTs?
In a recent “Perspective” article in The New England Journal of Medicine, three physicians (Drs. Cox, Borio, and Temple) make a strong case for not letting the rush to save Ebola patients tempt us to deviate from good science and skip the randomized controlled trial (RCT). Their arguments cut to the essence of the scientific approach to medicine, and they deserve careful...
Reflexology for Babies?
In the fascinating, if not rational, world of so-called complementary and alternative medicine, the age of the patient rarely seems to matter. This stands in stark contrast to the practice of science-based medicine. Sure, there is some physiological overlap across the spectrum of age, but caring for children often requires a vastly-different approach and there are numerous conditions not seen or only...

Hostility towards scientific consensus: A red flag identifying a crank or quack
Deniers of well-established science, such as the anthropogenic climate change, the theory of evolution, and vaccine science, frequently attack the scientific consensus. Some go farther and attack the very concept of a scientific consensus. When you see such attacks, you know you're dealing with a crank or, in the case of medicine, a quack.

