Category: Science and Medicine
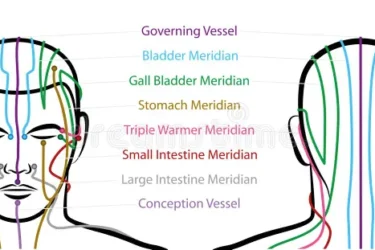
Science-Based Satire: TCM Experts Baffled by Man Born Without Meridians
Has the first case of complete congenital Qi deficiency been diagnosed in Massachusetts? Is it possible to run a successful landscaping business without any meridians? Where can you get acupuncture and your car detailed at the same time? All these questions and more will be answered in today's post, which I completely made up.

Quoth quacks, “The medical consensus has changed before, making my quackery science!”
Brave maverick doctors (i.e., quacks) have long tried to portray themselves as "innovators" challenging an ossified medical consensus for the good of patients. This tradition continues among COVID-19 quacks, in particular the Frontline COVID-19 Critical Care Alliance and its founders.

Vulnerable Children Really Count
Why were misinformation doctors so eager to spread the easily-refutable myth that "no healthy child" had died of COVID?
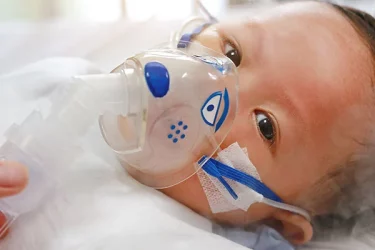
Nirsevimab is Great News for Infants, Caregivers, and Exhausted Pediatricians
RSV is a terrible infection that puts thousands of kids in the hospital every year and can be deadly. We will soon have a safe and effective way to prevent many of these severe cases, but it won't be easy to get shots into arms this season.

Sensible Medicine: Medical Misinformation and Medical Groupthink From the Medical Establishment
We all have biases, including in-group loyalty. It's often easy to see such bias in others, though nearly impossible to see in oneself. As such, it's both normal and dangerous to imagine that only those who disagree with you are vulnerable to groupthink, while you are perfect beacon of independent, rational thought- along with everyone who agrees with you.

The Grand Debunk of the antivaxxer book “Turtles All the Way Down” (part 4/10)
The debunking resumes with the fourth installment in debunking the antivaxxer book “Turtles All the Way Down”: Chapter 4, “Epidemiology 101," in which the antivax authors put a biased spin on basic concepts in epidemiology as a lead-in to their obviously intended purpose of claiming that all the studies finding vaccines to be safe and effective should be discounted.

Should Protein Powder Have a Warning Label?
The unfortunate death of a teen in London has some experts calling for new warning labels on products containing large amounts of protein. But would that work?

Conspirituality: A Book Recommendation
Conspirituality is a must-read for anyone who seeks to understand the daunting task we face in repairing the damage done by disinformation doctors.

The Grand Debunk of the antivaxxer book “Turtles All the Way Down” (part 3/10)
The third installment in debunking the antivaxxer book “Turtles All the Way Down”: Chapter 3, “Deficient by Design: The Vaccine Adverse Event Reporting System (VAERS)”.
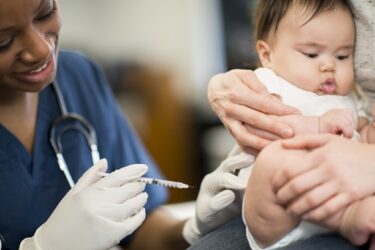
Childhood Vaccination Rates Move (Slowly) in the Right Direction
Childhood vaccination rates worldwide tanked during the first two years of the pandemic. A recently released report from the UN revealed that 2022 was better, but the improvements weren't seen everywhere. And we still have a long way to go.

