Category: Traditional Chinese Medicine

WHO Promotes Unscientific TCM
The World Health Organization endorses quackery in the form of TCM.

The Integrative Oncology Scholars Program: Indoctrinating the next generation of “integrative oncology” believers
"Integrative oncology" involves "integrating" pseudoscience, mysticism, and quackery with science-based oncology and co-opting science-based lifestyle modalities as "alternative" in order to provide cover for the quackery. Unfortunately, my alma mater, funded by the National Cancer Institute, is running a course to indoctrinate 100 health care professionals in the ways of "integrative oncology." The Trojan horse of "lifestyle interventions" and "nonpharmacologic treatments for...
World Health Organization Endorses Quackery
The World Health Organization fails its primary function by promoting traditional quackery.
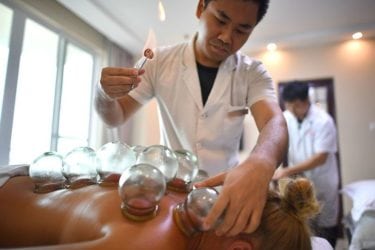
Acupuncture versus breast cancer treatment-induced joint pain: Spinning another essentially negative study
The investigators behind a recent clinical trial testing acupuncture to treat joint pain caused by aromatase inhibitors used to treat breast cancer are spinning it as a positive study. As is usually the case for acupuncture studies. It isn't

Confronting homeopathy, naturopathy, homeopathy, and other quackademic medicine at my alma mater
Several years back, I was forced to confront quackery at my alma mater in the form of an anthroposophic medicine program at the University of Michigan. The situation has deteriorated since then, as now the Department of Family Medicine there is inviting homeopaths to give talks and teaching acupuncture as credulously as any acupuncturist. Will the disease metastasize to other departments in...

So-Called Alternative Medicine
Edzard Ernst calls it "So-Called Alternative Medicine". This insider's view of SCAM is a new book from an prolific researcher and author.

Science-based medicine versus other ways of knowing
It has been our position that science is the most effective means of determining medical treatments that work and whose benefits outweigh their risks. Those who promote pseudoscientific or prescientific medicine, however, frequently appeal to other ways of knowing, often ancient knowledge from other cultures and pointing out deficiencies in SBM to justify promoting their treatments. Do their justifications hold water?

Bee Venom is Snake Oil
Bee venom acupuncture is a double-barrel pseudoscience that provides new example of an old problem - the use of poor quality preclinical research to justify the inclusion of nonsense in medicine.

Another pebble in the quackademic integrative avalanche
We've documented the infiltration of quackery into academic medicine through the "integration" of mystical and prescientific treatment modalities into medicine. Here, we look at a pebble in the quackademic avalanche. Is it too late for the pebbles to vote?

ICD-11: A triumph of the “integration” of quackery with real medicine
ICD-10 is an a standardized system of alphanumeric codes for diagnoses maintained by the World Health Organization used throughout the world for billing, epidemiology, research, and cataloging causes of death. Its successor, ICD-11, is nearing completion, and unfortunately appears to be taking the "integration" of traditional medicine to a whole new level by integrating quack diagnoses with real diagnoses.

