Category: Vaccines
The risks associated with alternative medicine
In a new paper, the types and severity of harms from different types of alternative medicine are described.
The Delta Variant
The emergence of the delta variant of SARS-CoV-2, leading to more cases of COVID-19, is a reminder that we have not won this race against the pandemic yet.

“Depopulation” by COVID-19 vaccines?
COVID-19 and antivaccine conspiracy theorists like Joe Mercola, Michael Yeadon, and Peter McCullough are spreading the conspiracy theory that COVID-19 vaccines are intended as a tool for "global depopulation". This is nothing more than an old antivaccine conspiracy theory repurposed for the pandemic. As ridiculous as it might seem, it is nonetheless very appealing to antivaxxers.
“COVID-19 vaccines are going to sterilize our womenfolk,” Take 2
Antivaxxers have long claimed that vaccines, particularly HPV vaccines, can damage the ovaries and cause female infertility. That claim has been resurrected for COVID-19 vaccines. The first example relied on a dubious "similarity" between the SARS-CoV-2 spike protein and a placental protein. This time, it's the lipid nanoparticles attacking the ovaries, echoing very old claims about polysorbate-80. Truly, everything old is new...
Legislatures and litigation: anti-vaxxers continue attacks on COVID mitigation
Anti-vaxxers are attacking COVID-19 mandates in state legislatures and in court even as COVID-19 cases numbers and hospitalizations remain high among the unvaccinated.
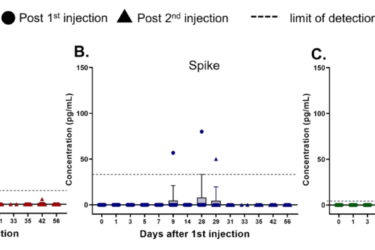
The “deadly” coronavirus spike protein (according to antivaxxers)
Antivaxxers are citing three papers to support their claim that spike protein produced by COVID-19 vaccines is dangerous. Unsurprisingly and as usual, they're misinterpreting the studies and misrepresenting their significance. COVID-19 vaccines are, in fact, very safe.
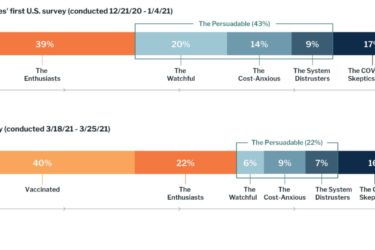
The Causes of Vaccine Hesitancy
The vaccine hesitant are now the front lines of the battle to contain COVID.
Should COVID-19 vaccines be administered to children under an emergency use authorization?
Recently, Wesley Pegden, Vinay Prasad, and Stefan Baral argued in The BMJ that "COVID-19 vaccines for children should not get emergency use authorization". Their argument is lacking, and they left out a number of relevant facts.

The COVID-19 “Vaccine Holocaust”: The latest antivaccine messaging
The latest antivaccine disinformation consists of pointing to the large numbers of reports of death (and other adverse events) to the VAERS database. It's nonsense.
COVID vaccine manufacturers should explore legal action against anti-vaxxers spreading disinformation
Perhaps it's time for vaccine manufacturers to consider defamation suits against anti-vaxxers who spread false information about COVID vaccines. Lawsuits by voting technology companies against Fox and others over false "rigged" election claims could serve as a template.

