J.B. Handley versus vaccine science. Again. Not surprisingly, J.B. loses.
Our old friend anti antivaccine activist J. B. Handley invokes the "vaccines didn't save us" gambit. It doesn't go well for him.

A London Chiropractor Gets His Undeserved Fifteen Minutes of Fame
Thanks to his anti-science and anti-medicine worldview, and a complete misunderstanding of evolution, a London chiropractor is getting some undeserved attention from the media.
Brief Announcement: SkepDoc’s Website
I have a newly-revamped website!

Open thread: The floor is yours
What topics do you want to see addressed by SBM's contributors? The floor is yours today.

No Benefit from Fish Oil
A new systematic review of clinical trials shows no clear benefit to consuming omega-3 fatty acids in food or supplements.
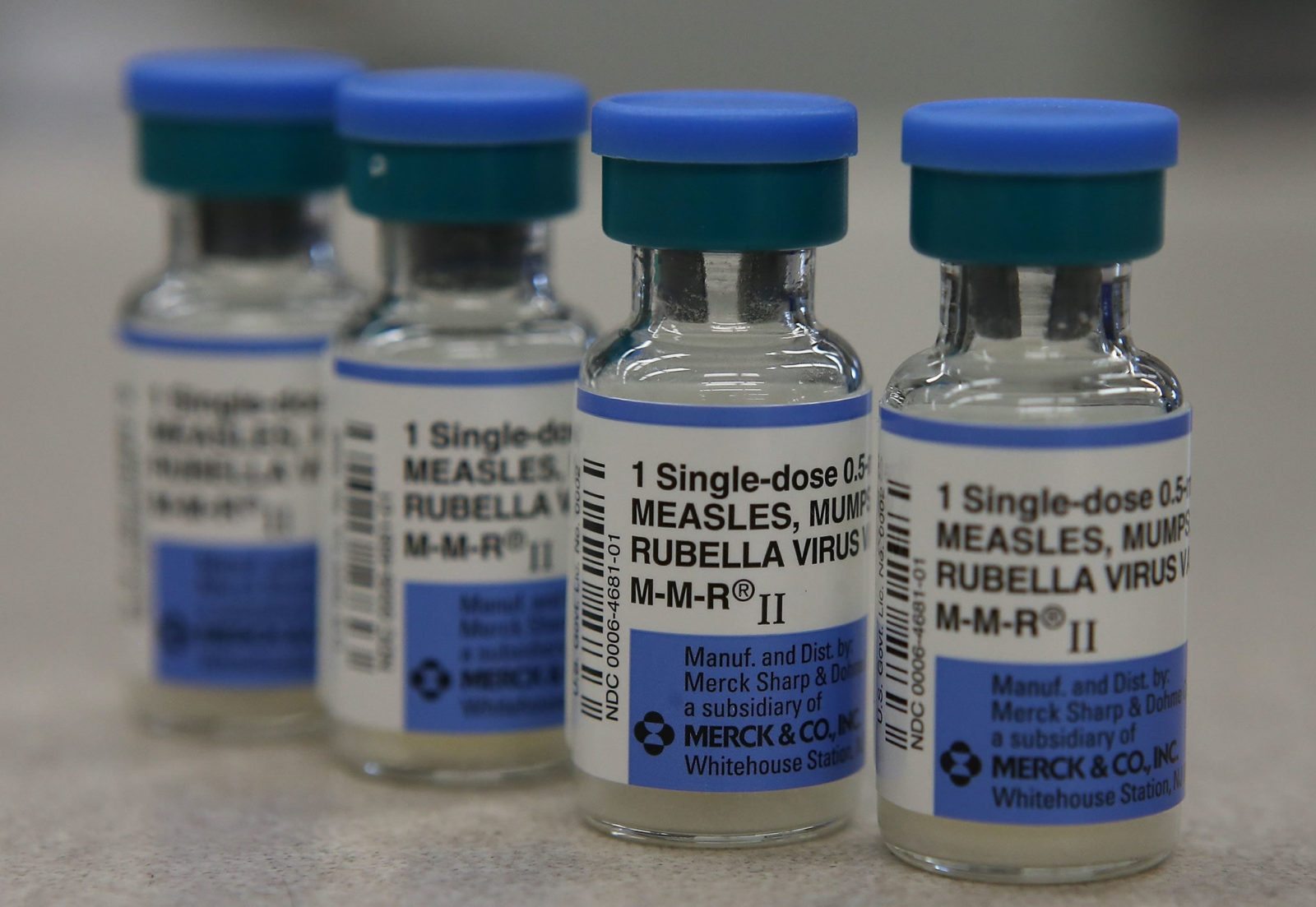
Are antivaxers “holding science hostage”?
Melinda Wenner Moyer published an article in The New York Times arguing that fear of how antivaxers will react to scientific findings is leading scientists to self-censor. I'm not convinced that this is the case.

Double standards in hematology for integrative and complementary medicine: a case study
In this post I discuss several yoga studies that were presented to a gathering of some of the world’s best MPN researchers and clinicians. They illustrate an apparent double standard in hematological cancer research, which allows integrative and complementary treatments to skip over the normally high rigor and standards typical of the sub-specialty.

FDA blacklists cesium chloride, ineffective and dangerous naturopathic cancer treatment
The FDA recently issued an alert warning of significant safety risks associated with cesium chloride. It is a mineral salt promoted by naturopathic “doctors” and “integrative” medicine practitioners as an alternative treatment for cancer, despite the lack of evidence of safety and efficacy in treating cancer or any other disease.

Electromagnetic Fields at Work Show No Brain Tumor Risk
A new study finds no significant correlation between workplace exposure to radio frequency (RF) or intermediate frequency (IF) electromagnetic waves and the most common brain tumors. This is more reassuring evidence that non-ionizing EMFs are probably safe.